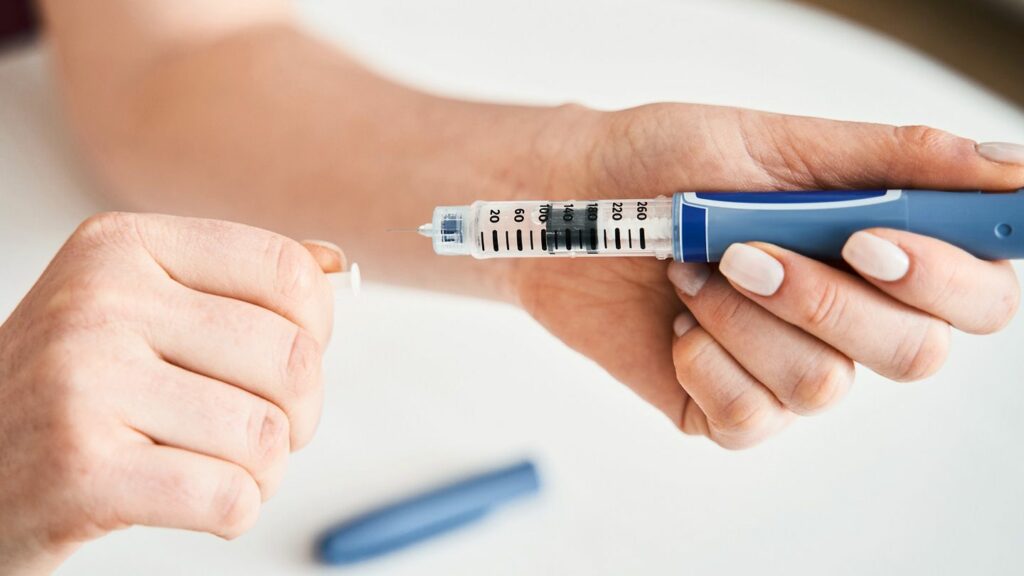
While insulin injections are a well-known and widely used treatment, there is a diverse array of non-insulin injectables that play a crucial role in diabetes care. In this blog, we’ll delve into the world of non-insulin injectables, exploring their mechanisms, benefits, and how they contribute to effective diabetes management. Whether you’re newly diagnosed or seeking alternative treatment options, understanding the range of injectables available can empower you to make informed decisions about your health.
Contents
What Are Injectable Non-Insulin Drugs?
 Injectable non-insulin drugs are a class of medications designed to assist individuals with diabetes in managing their blood glucose levels. Unlike insulin injections, which are a well-known and primary treatment for diabetes, non-insulin injectables employ various mechanisms to regulate blood sugar. One prominent category is GLP-1 receptor agonists. This mimics the action of a naturally occurring hormone, glucagon-like peptide-1 (GLP-1).
Injectable non-insulin drugs are a class of medications designed to assist individuals with diabetes in managing their blood glucose levels. Unlike insulin injections, which are a well-known and primary treatment for diabetes, non-insulin injectables employ various mechanisms to regulate blood sugar. One prominent category is GLP-1 receptor agonists. This mimics the action of a naturally occurring hormone, glucagon-like peptide-1 (GLP-1).
These drugs stimulate insulin release, suppress glucagon secretion, and slow down gastric emptying, collectively working to lower blood sugar levels. Another significant group is SGLT-2 inhibitors, which target the sodium-glucose cotransporter-2 in the kidneys, leading to increased glucose excretion in urine. By harnessing different physiological pathways, non-insulin injectables offer additional options for diabetes management beyond traditional insulin therapy.
These injectable medications are often prescribed when lifestyle changes and oral medications alone are insufficient to control blood glucose levels. They play a crucial role in providing personalized and effective treatment options for individuals with diabetes. And, offering alternatives for those who may face challenges with insulin therapy or seek additional strategies to enhance glycemic control.
What Are Some Examples Of Non-Insulin Injectables?
Several non-insulin injectables are available for the management of diabetes, offering diverse options to individuals who may not be using or responding well to insulin therapy. Some notable examples include:
GLP-1 Receptor Agonists
GLP-1 receptor agonists are a class of non-insulin injectables that mimic the action of the natural hormone glucagon-like peptide-1 (GLP-1). Exenatide (Byetta, Bydureon) and liraglutide (Victoza, Saxenda) are examples of medications in this category. Byetta and Bydureon are injectable medications that need to be administered before meals.
And, promote insulin release, suppress glucagon secretion, and slow down the emptying of the stomach. Liraglutide, on the other hand, offers dual benefits by managing blood sugar levels in diabetes (Victoza) and aiding in weight management (Saxenda).
SGLT-2 Inhibitors
Sodium-glucose cotransporter-2 (SGLT-2) inhibitors, such as canagliflozin (Invokana), dapagliflozin (Farxiga), and empagliflozin (Jardiance), represent another class of non-insulin injectables. These medications work by inhibiting SGLT-2 in the kidneys, reducing the reabsorption of glucose, and promoting its excretion through urine. Canagliflozin, dapagliflozin, and empagliflozin are known for their ability to lower blood sugar levels, and they have shown additional cardiovascular benefits.
Amylin Analogs
Pramlintide (Symlin) is an injectable medication classified as an amylin analog. Administered alongside insulin, pramlintide works by mimicking the action of amylin, a hormone that is deficient in individuals with diabetes. By slowing down gastric emptying, reducing glucagon secretion, and enhancing feelings of satiety, pramlintide helps control post-meal blood sugar levels. This injectable is especially useful for those who experience significant postprandial glucose spikes despite insulin therapy.
Combination Therapies
 Some non-insulin injectables come in combination formulations, combining different classes of medications to enhance their effectiveness. For instance, dulaglutide and liraglutide are available in combination with basal insulin in products like Xultophy and Soliqua. These combinations offer the benefits of both GLP-1 receptor agonists and insulin in a single injection, addressing both short- and long-term blood sugar control needs. This approach simplifies the treatment regimen for individuals with diabetes, providing a convenient option that can potentially improve adherence and overall diabetes management.
Some non-insulin injectables come in combination formulations, combining different classes of medications to enhance their effectiveness. For instance, dulaglutide and liraglutide are available in combination with basal insulin in products like Xultophy and Soliqua. These combinations offer the benefits of both GLP-1 receptor agonists and insulin in a single injection, addressing both short- and long-term blood sugar control needs. This approach simplifies the treatment regimen for individuals with diabetes, providing a convenient option that can potentially improve adherence and overall diabetes management.
It’s important to note that the availability of these medications may vary by region, and healthcare providers will tailor the treatment plan based on individual patient needs medical history, and specific requirements for diabetes management. Always consult with a healthcare professional for personalized advice and guidance on medication choices.
What Is The Dosage Recommendation?
The dosage recommendations for non-insulin injectables can vary based on the specific drug, the individual’s health status, and the treatment goals. Here is a general overview of dosages for some common non-insulin injectables:
1. GLP-1 Receptor Agonists
- Exenatide (Byetta, Bydureon): Typically, Byetta is injected twice daily before meals, while Bydureon is a once-weekly injection.
- Liraglutide (Victoza, Saxenda): For diabetes management, Victoza is usually administered once daily, while Saxenda, used for weight management, may have a different dosing schedule.
- Dulaglutide (Trulicity): Administered once weekly.
2. SGLT-2 Inhibitors
- Canagliflozin (Invokana), dapagliflozin (Farxiga), and empagliflozin (Jardiance): Typically, these medications are taken orally rather than by injection. The dosage will be specified by the prescribing healthcare professional.
3. Amylin Analogs
- Pramlintide (Symlin): Dosage recommendations for pramlintide will depend on the individual’s insulin regimen and specific needs. It is usually injected before meals in addition to insulin.
4. Combination Therapies
- Combination products like Xultophy and Soliqua, which include GLP-1 receptor agonists and basal insulin, have specific dosing schedules. These are typically administered once daily.
It’s crucial to note that dosages may be adjusted over time based on factors such as blood glucose monitoring results, changes in health status, or any observed side effects. Never adjust the dosage of any medication without consulting a healthcare professional, as doing so could lead to inadequate blood sugar control or other complications.
What Are The Side Effects of Non-Insulin Injectables?
 The side effects of non-insulin injectable medications can vary depending on the specific class of drug. Here are some common side effects associated with non-insulin injectables, without mentioning specific medication names:
The side effects of non-insulin injectable medications can vary depending on the specific class of drug. Here are some common side effects associated with non-insulin injectables, without mentioning specific medication names:
- Gastrointestinal Distress
Many non-insulin injectables, particularly GLP-1 receptor agonists, may cause gastrointestinal side effects such as nausea, vomiting, diarrhea, or constipation. These symptoms often occur during the initial weeks of treatment and may improve over time.
- Hypoglycemia
While non-insulin injectables are less likely to cause hypoglycemia (low blood sugar) compared to insulin, some individuals may still experience this side effect. Especially when these medications are used in combination with other glucose-lowering agents.
- Genitourinary Infections
SGLT-2 inhibitors, which work by promoting the excretion of glucose in urine, may increase the risk of genital and urinary tract infections. Patients should be aware of symptoms such as itching, burning, or pain and seek medical attention if these occur.
- Injection Site Reactions
Injectable medications may occasionally cause mild irritation or reactions at the injection site, such as redness, swelling, or discomfort. Rotating injection sites and proper technique can help minimize these reactions.
- Weight Changes
GLP-1 receptor agonists may be associated with weight loss, which can be a desired effect for individuals with diabetes who are overweight. However, weight loss may vary among individuals.
- Pancreatitis
There is a rare but serious risk of pancreatitis associated with some non-insulin injectables. Symptoms include severe abdominal pain that may radiate to the back. Individuals experiencing such symptoms should seek prompt medical attention.
Individuals need to be aware of potential side effects and promptly report any concerns to their healthcare provider. These side effects are not exhaustive. The actual side effect profile can vary based on the specific medication, individual health factors, and overall treatment plan.
Conclusion
In conclusion, exploring the world of non-insulin injectables reveals a diverse range of medications that offer valuable alternatives for managing diabetes. From GLP-1 receptor agonists to SGLT-2 inhibitors and amylin analogs, these injectables provide tailored solutions to help regulate blood glucose levels. They cater to individuals seeking effective options beyond insulin therapy, offering benefits such as weight management and reduced risk of hypoglycemia.
Personalized treatment plans, combination therapies, and ongoing advancements in research highlight the evolving landscape of diabetes care. By understanding the nuances of non-insulin injectables, individuals with diabetes can engage in informed discussions with healthcare providers. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.