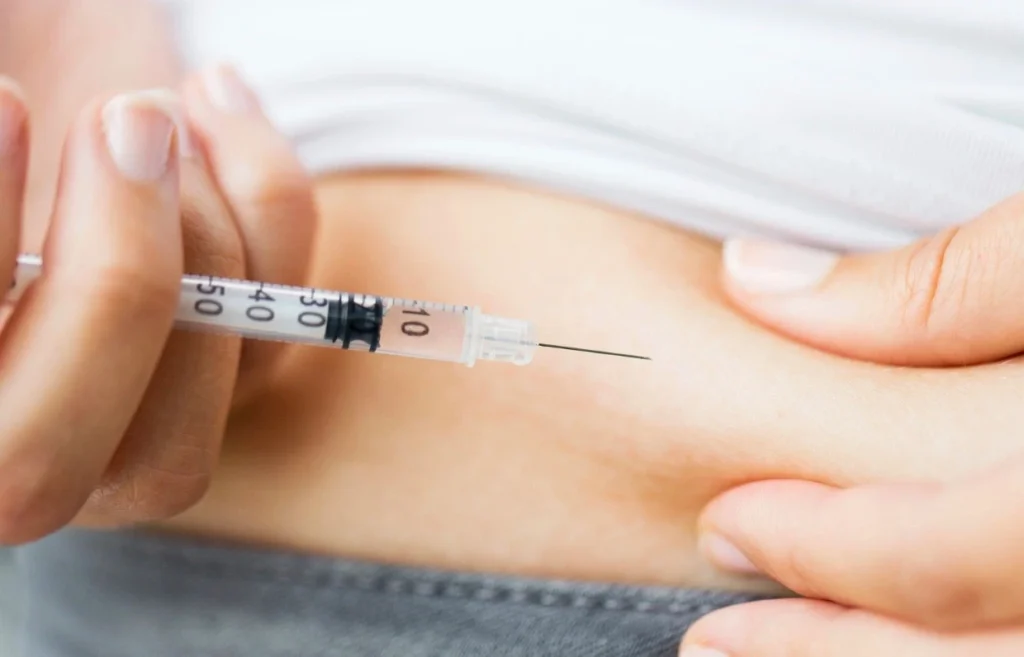
Insulin therapy is a critical component in the management of diabetes, a condition that affects millions of people worldwide. The purpose of insulin therapy is to mimic the body’s natural insulin production, thus regulating blood glucose levels and preventing complications associated with diabetes. This guide aims to provide a thorough overview of insulin therapy, discussing its various forms, administration techniques, and vital role in diabetes management.
Contents
When Is Insulin Therapy Used?
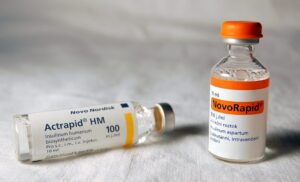 Insulin therapy is used primarily in the treatment of diabetes, a chronic condition where the body is unable to properly regulate blood sugar (glucose) levels. The specific scenarios in which insulin therapy is employed include:
Insulin therapy is used primarily in the treatment of diabetes, a chronic condition where the body is unable to properly regulate blood sugar (glucose) levels. The specific scenarios in which insulin therapy is employed include:
- Type 1 Diabetes
In this condition, the body’s immune system destroys the cells in the pancreas that produce insulin. Individuals with type 1 diabetes require insulin therapy from the time of diagnosis.
- Type 2 Diabetes
People with type 2 diabetes may need insulin therapy if other treatments, such as lifestyle changes and oral medications, are not enough to control their blood glucose levels. Insulin therapy in type 2 diabetes is often a later-stage treatment when the pancreas is no longer able to produce sufficient insulin to overcome insulin resistance.
- Gestational Diabetes
This form of diabetes occurs during pregnancy and may require insulin therapy if blood sugar levels cannot be controlled by diet and exercise alone. Insulin is preferred over oral medications in pregnancy because it does not cross the placenta and therefore is safer for the developing fetus.
- Diabetic Ketoacidosis (DKA)
This is a serious complication of diabetes that occurs predominantly in type 1 diabetes but can also occur in type 2. It requires immediate medical attention and the administration of insulin, along with fluids and electrolytes.
- During Surgery or Acute Illness
In situations of stress, such as surgery or acute illness, even people with type 2 diabetes who usually manage their condition with diet and oral medications may temporarily require insulin to keep their blood sugar levels under control.
The decision to start insulin therapy is individualized and based on several factors. This therapy requires careful monitoring and regular adjustments by healthcare professionals in collaboration with the patient.
How Do You Start Insulin Therapy?
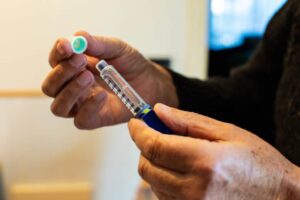 Starting insulin therapy is a significant step in diabetes management, and it involves several key steps to ensure safety and effectiveness. Here’s a general outline of how insulin therapy is typically initiated:
Starting insulin therapy is a significant step in diabetes management, and it involves several key steps to ensure safety and effectiveness. Here’s a general outline of how insulin therapy is typically initiated:
Medical Evaluation
Before starting insulin therapy, a comprehensive medical evaluation is necessary. This includes assessing your current diabetes management, blood sugar control, any complications of diabetes, and overall health status. The healthcare provider will consider factors like your lifestyle, eating habits, and other medications you are taking.
Type of Insulin
Depending on the type of diabetes and individual needs, the doctor will choose the most appropriate type of insulin. This could be rapid-acting, short-acting, intermediate-acting, or long-acting insulin or a combination of these.
Dosage Determination
The initial insulin dose is typically conservative to minimize the risk of hypoglycemia (low blood sugar). The doctor will guide how much insulin to take and when to take it. The dosage may be adjusted over time based on blood sugar monitoring results.
Instruction on Insulin Administration
Patients receive detailed instructions on how to administer insulin. This includes choosing an injection site (such as the abdomen, thigh, or upper arm), rotating the sites, and the technique of injecting. Training may also be provided for using insulin pens, syringes, or pumps.
Blood Sugar Monitoring
Frequent blood sugar monitoring is essential when starting insulin therapy. This helps in understanding how your body responds to insulin and in making necessary dose adjustments. It also helps in identifying and managing hypoglycemia.
Regular Follow-up and Adjustment
Regular follow-up appointments are necessary to monitor progress, address any issues, and adjust insulin doses as needed. This includes reviewing blood sugar logs and discussing any side effects or concerns.
Safety and Emergency Protocols
Patients are educated about safety protocols, including proper storage of insulin and how to manage diabetes during illness or stress.
It’s important to remember that starting insulin therapy is a highly individualized process, and what works best for one person may not be the same for another. Ongoing communication with healthcare professionals is key to successfully managing diabetes with insulin therapy.
What Are The Types Of Insulin?
Insulin is available in several different types, each varying in how quickly it starts to work (onset), when it reaches its peak effectiveness (peak time), and how long it lasts (duration). The types of insulin are typically categorized based on these characteristics. Here’s an overview:
Rapid-Acting Insulin
- Onset: Begins to work within 15 minutes.
- Peak: Peak around 1 to 2 hours after injection.
- Duration: Last for 3 to 5 hours.
- Examples: Insulin lispro (Humalog), insulin aspart (NovoLog, Fiasp), and insulin glulisine (Apidra).
- Usage: Taken just before or with a meal to cover the rise in blood sugar that comes with eating.
Short-acting insulin (Regular or R Insulin)
- Onset: Starts working within 30 minutes.
- Peak: Peak around 2 to 3 hours after injection.
- Duration: Last approximately 6 to 8 hours.
- Examples: Regular Human Insulin (Humulin R, Novolin R).
- Usage: Usually taken about 30 minutes before a meal.
Intermediate-Acting Insulin
- Onset: Begins to work within 1 to 3 hours.
- Peak: Peak in about 8 hours and can last up to 16 hours.
- Duration: Covers insulin needs for about half the day or overnight.
- Examples: NPH (Neutral Protamine Hagedorn) insulin, such as Humulin N, Novolin N.
- Usage: Often combined with rapid- or short-acting insulin.
Long-Acting Insulin
- Onset: Starts working several hours after injection.
- Peak: Provides a steady insulin level; some forms do not have a pronounced peak.
- Duration: Can last up to 24 hours or more.
- Examples: Insulin glargine (Lantus, Basaglar, Toujeo), insulin detemir (Levemir), insulin degludec (Tresiba).
- Usage: Provides a constant level of insulin to manage blood sugar between meals and overnight.
Ultra-Long-Acting Insulin
- Onset: Starts working in 6 hours or more.
- Peak: Very stable and peakless profile.
- Duration: Lasts over 36 hours, providing more stable insulin action over a longer period.
- Example: Insulin degludec (Tresiba).
- Usage: For those who need a very steady insulin level and have a varying schedule.
Pre-Mixed Insulin
- Composition: Combination of intermediate-acting and short- or rapid-acting insulin in one bottle or an insulin pen.
- Usage: Typically taken twice a day before meals; useful for people who have difficulty mixing insulins.
Each type of insulin is designed to mimic the way natural insulin works in people without diabetes. Healthcare professionals will help determine the best insulin regimen for each person, often using a combination of different types to manage blood sugar.
What Are The Benefits And Side Effects Of Insulin Therapy?
 Insulin therapy is a cornerstone in the management of diabetes, particularly for individuals with type 1 diabetes and for many with type 2 diabetes. It provides significant benefits but also comes with potential side effects.
Insulin therapy is a cornerstone in the management of diabetes, particularly for individuals with type 1 diabetes and for many with type 2 diabetes. It provides significant benefits but also comes with potential side effects.
Benefits
- Blood Sugar Control: The primary benefit of insulin therapy is its ability to lower and regulate blood sugar levels, helping to keep them within a target range. This reduces the symptoms of high blood sugar and decreases the risk of complications.
- Reduction of Complications: Long-term, consistent blood sugar management can significantly reduce the risk of complications associated with diabetes, such as heart disease, kidney failure, nerve damage, vision problems, and stroke.
- Flexibility in Diet and Lifestyle: Insulin therapy can offer more flexibility in terms of diet and lifestyle compared to oral diabetes medications. It allows for adjustments in insulin dosing to accommodate changes in eating habits, physical activity, and stress levels.
- Improved Energy and Well-being: Effective insulin therapy helps in stabilizing blood sugar levels, which can lead to improved energy levels and overall well-being.
- Versatility: Different types of insulin can be used to manage unique individual needs and lifestyles, offering a personalized approach to diabetes care.
Side Effects
- Hypoglycemia (Low Blood Sugar): This is the most common and potentially serious side effect. Symptoms include shakiness, confusion, sweating, hunger, and, in severe cases, loss of consciousness.
- Weight Gain: Some people may experience weight gain when they start using insulin. This can be managed with dietary adjustments and regular physical activity.
- Lipodystrophy: Repeated insulin injections at the same site can cause changes in fat tissue, leading to lumps (lipohypertrophy) or dents (lipoatrophy) in the skin.
- Allergic Reactions: Though rare with modern insulin formulations, some people may experience allergic reactions at the injection site or systemically.
- Swelling or Fluid Retention: Some individuals may notice swelling in their extremities or mild fluid retention when they start insulin therapy.
- Insulin Resistance: Over time, some individuals might require higher doses of insulin due to increased resistance, particularly in type 2 diabetes.
Managing these side effects often involves adjusting insulin dosage, altering injection sites, dietary changes, and increased monitoring of blood sugar levels. Regular education and self-care practices are crucial in managing diabetes effectively with insulin therapy.
Conclusion
In conclusion, insulin therapy is a vital tool in effectively managing diabetes and improving the quality of life for millions worldwide. By regulating blood sugar levels, this therapy helps to prevent complications. While it offers numerous benefits, including flexibility in lifestyle and personalized treatment options, it’s essential to be aware of potential side effects.
With proper education, support from healthcare professionals, and diligent self-care practices, individuals can navigate insulin therapy successfully. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.