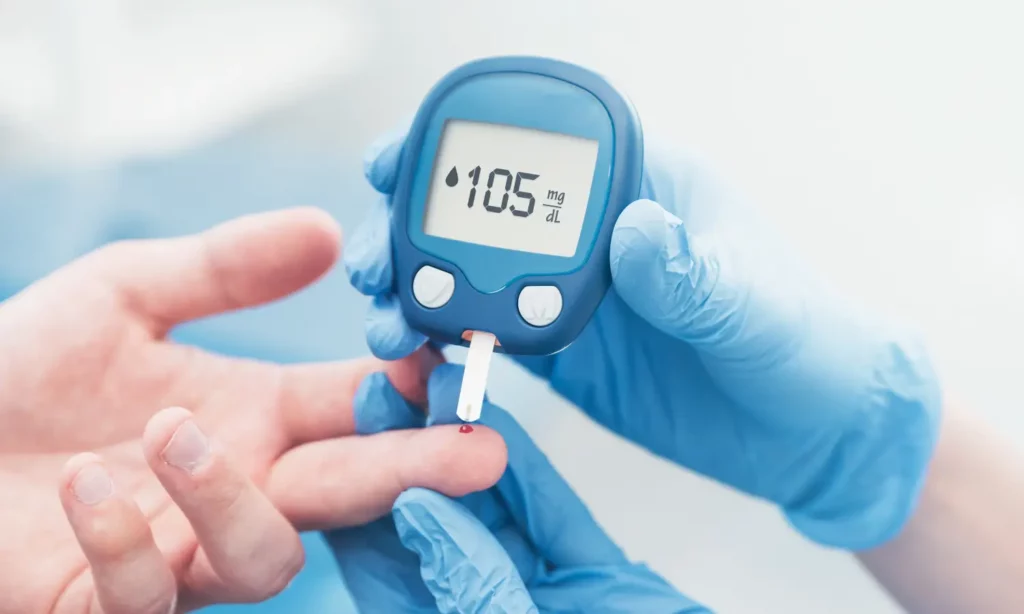
Insulin resistance, a very complex condition, if not detected early, can even end up making you diabetic! It’s when your body doesn’t respond to insulin, a crucial hormone produced by your pancreas. This hormone is responsible for regulating blood sugar levels. But if your body fails to respond to insulin, it can cause diabetes. Well, without any further ado, let’s get into the details of this topic. In this blog, you’ll get to know about the signs and symptoms of insulin resistance, its causes, and most importantly, some effective treatment options and ways to reverse it. So, let’s get started!
Contents
- 1 What Is Insulin Resistance?
- 2 Does Having Insulin Resistance Mean I Have Diabetes?
- 3 Assess Your Risk: Diabetes Risk Test
- 4 Signs, Symptoms, and Causes of Insulin Resistance
- 5 Risk Factors Associated With Insulin Resistance
- 6 Treatment To Manage Insulin Resistance
- 7 Healthy Diet for Insulin Resistance
- 8 Conclusion
What Is Insulin Resistance?
In simple terms, insulin resistance occurs when your body’s cells fail to respond adequately to the insulin produced. Insulin is a hormone produced by the pancreas, essential for regulating blood sugar levels. It acts as a key, unlocking cells to allow glucose entry, and promoting energy utilization and storage. To comprehend this, let’s break down the process.
- Your body breaks down the food you consume into glucose, which serves as the primary energy source.
- This glucose enters your bloodstream, prompting the pancreas to release insulin.
- Insulin facilitates the entry of glucose into muscle, fat, and liver cells, enabling them to use it for energy or store it for future use.
However, due to various factors, your cells may respond inappropriately to insulin. Consequently, they struggle to efficiently absorb glucose from the bloodstream or store it, giving rise to the condition known as insulin resistance.
Does Having Insulin Resistance Mean I Have Diabetes?
 Having insulin resistance does not automatically equate to a diabetes diagnosis. Here’s the crucial distinction: as long as your pancreas can produce sufficient insulin to compensate for your cells’ weakened response, your blood sugar levels will remain within a normal range.
Having insulin resistance does not automatically equate to a diabetes diagnosis. Here’s the crucial distinction: as long as your pancreas can produce sufficient insulin to compensate for your cells’ weakened response, your blood sugar levels will remain within a normal range.
However, a critical shift occurs when your cells become excessively resistant to insulin. This leads to a notable consequence, and it results in elevated blood glucose levels, a condition known as hyperglycemia.
Over time, sustained hyperglycemia becomes a precursor to more serious conditions. This means prolonged insulin resistance can evolve into prediabetes and eventually manifest as Type 2 diabetes.
Understanding this progression is vital for early intervention and proactive health management, emphasizing the importance of monitoring insulin sensitivity to prevent the onset of more severe metabolic conditions.
Assess Your Risk: Diabetes Risk Test
Before we move further, take a moment to assess your risk of diabetes by completing the Diabetes Risk Test available at Diabetes Mantra. This simple yet insightful test provides a personalized evaluation of your diabetes risk based on various factors.
Signs, Symptoms, and Causes of Insulin Resistance

If you have insulin resistance and observe an increase in your blood sugar levels, it’s crucial to be vigilant about potential signs and symptoms of diabetes. Early detection is key, as it signifies that insulin may not be functioning effectively. Here are some indicators of elevated blood sugar:
Signs of High Blood Sugar:
- Unexplained thirst could be a signal of elevated blood sugar levels.
- The need for frequent urination may indicate an imbalance in blood sugar.
- Persistent hunger, especially shortly after meals, can be a sign of insulin resistance.
- Vision changes, particularly blurriness, may be linked to elevated blood sugar.
- Recurrent headaches may be a symptom of fluctuating blood sugar levels.
- Increased susceptibility to infections in the vaginal and skin areas.
- Delayed healing of cuts and sores may be indicative of compromised blood sugar regulation.
Additional Risk Factors:
- Excessive Fat: A waistline measuring over 40 inches in men and 35 inches in women can contribute to insulin resistance.
- Elevated levels of triglycerides or cholesterol are additional risk factors.
- High Blood Pressure: Hypertension is linked to insulin resistance and should be monitored closely.
Understanding the causes of insulin resistance is equally essential. While there is much to uncover about its precise development, scientists identify two primary contributing factors:
Causes of Insulin Resistance
- Excess Body Fat
- Physical Inactivity
In summary, vigilant monitoring of blood sugar levels and recognizing associated signs and symptoms is crucial for early diagnosis and intervention. Additionally, addressing contributing factors such as excess body fat and promoting physical activity are fundamental steps towards mitigating the risks associated with insulin resistance.
Risk Factors Associated With Insulin Resistance

Identifying and understanding the risk factors associated with insulin resistance is imperative for proactive health management. Let’s delve into the key risk factors:
- Genetic Predisposition: A family history of insulin resistance or Type 2 diabetes increases the likelihood of developing insulin resistance.
- Sedentary Lifestyle: Lack of physical activity and prolonged periods of sitting contribute significantly to insulin resistance. Regular exercise is crucial for maintaining insulin sensitivity.
- Unhealthy Dietary Habits: Consuming a diet high in refined sugars, processed foods, and saturated fats can contribute to insulin resistance. A balanced and nutritious diet is vital for metabolic health.
- Excess Body Weight: Obesity, particularly the accumulation of visceral fat around the abdomen, is a major risk factor for insulin resistance. Maintaining a healthy weight is pivotal in reducing this risk.
- Age: As individuals grow older, a proactive approach to lifestyle choices becomes increasingly crucial.
- Hormonal Factors: Hormonal imbalances, such as those associated with conditions like polycystic ovary syndrome (PCOS), can contribute to insulin resistance.
- Medical Conditions: Certain medical conditions, such as hypertension and cardiovascular diseases, are linked to insulin resistance.
- Sleep Deprivation: Inadequate or poor-quality sleep has been identified as a risk factor for insulin resistance.
- Smoking: Tobacco smoke contains chemicals that can interfere with insulin activity, increasing the risk of insulin resistance.
- Stress: Chronic stress can elevate cortisol levels, negatively impacting insulin sensitivity. Stress management strategies are integral for overall health.
Understanding these risk factors empowers individuals to make informed lifestyle choices, minimizing the likelihood of developing or exacerbating insulin resistance. Proactive measures, including regular physical activity, a balanced diet, and maintaining a healthy weight, play pivotal roles in mitigating these risks and promoting long-term metabolic health.
Treatment To Manage Insulin Resistance
Yes, it’s possible to reverse insulin resistance, a proactive measure that significantly decreases the chances of developing prediabetes and Type 2 diabetes. Understanding the treatment modalities is key to empowering individuals in their journey towards managing insulin resistance.
Regular Exercise
 Engaging in regular physical activity is a cornerstone in the reversal of insulin resistance. Committing to half an hour of exercise 3–5 days per week can yield immediate benefits by enhancing insulin sensitivity. Aerobic exercises, strength training, and a combination of both contribute to overall metabolic well-being.
Engaging in regular physical activity is a cornerstone in the reversal of insulin resistance. Committing to half an hour of exercise 3–5 days per week can yield immediate benefits by enhancing insulin sensitivity. Aerobic exercises, strength training, and a combination of both contribute to overall metabolic well-being.
Eat A Healthy Diet

Transforming dietary habits plays a pivotal role in combating insulin resistance. Incorporate the following into your diet:
- Colorful Fruits and Vegetables
Opt for a diverse array of fruits and vegetables, as their vibrant colors often signify rich nutritional content. - Fiber-Rich Foods
Include high-fiber foods like whole grains, legumes, and nuts, promoting stable blood sugar levels. - Healthy Fats
Embrace sources of healthy fats, such as avocados, nuts, and olive oil, which contribute to improved insulin sensitivity. - Lean Proteins
Prioritize lean protein sources like poultry, fish, and plant-based proteins.
Reduce Weight
For individuals with excess body weight, weight reduction is a powerful strategy for reversing insulin resistance. Achieving and maintaining a healthy weight positively impacts insulin sensitivity and overall metabolic function.
Medications
 In some cases, healthcare professionals may recommend medications to complement lifestyle changes. Commonly prescribed medications include:
In some cases, healthcare professionals may recommend medications to complement lifestyle changes. Commonly prescribed medications include:
- Metformin: Often the initial choice, metformin enhances insulin sensitivity, facilitating the entry of glucose into cells and reducing glucose production by the liver.
- Pioglitazone (Actos) and Rosiglitazone (Avandia): These medications assist cells in using insulin more effectively and decrease glucose production by the liver.
Disclaimer: Medications should only be taken as prescribed by a qualified healthcare professional. Consultation with your healthcare provider is paramount to ensure the appropriateness and safety of any prescribed medications for your specific health condition.
Healthy Diet for Insulin Resistance
 Your diet plays a pivotal role in influencing blood sugar and insulin levels, making informed dietary choices crucial for managing and reversing insulin resistance. Opting for a diet that focuses on low to medium-glycemic index foods while incorporating fiber-rich options can significantly impact your metabolic health.
Your diet plays a pivotal role in influencing blood sugar and insulin levels, making informed dietary choices crucial for managing and reversing insulin resistance. Opting for a diet that focuses on low to medium-glycemic index foods while incorporating fiber-rich options can significantly impact your metabolic health.
- Avoid Processed and High-Carbohydrate Foods
Highly processed, high-carbohydrate, and high-fat foods often demand increased insulin production. Minimizing their consumption is vital for managing insulin resistance. - Low to Medium Glycemic Index Foods
Choosing foods with a low to medium glycemic index aids in stabilizing blood sugar levels. This includes:- Dark Green, Leafy Veggies (e.g., Spinach): Low in carbs and calories, these nutrient-packed vegetables offer an excellent choice for regulating blood sugar.
- Fruits (e.g., Avocados, Apples, Berries): Packed with vitamins, minerals, and fiber, these fruits contribute to a balanced and diabetes-friendly diet.
- High Fiber Intake
Foods rich in fiber help regulate blood sugar levels by slowing down the digestion process. This prevents rapid spikes in blood sugar. Incorporate:- Legumes (e.g., Lentils): High in fiber, legumes are a great choice for managing insulin resistance.
- Whole Grains: Opt for whole grains to provide sustained energy and support stable blood sugar levels.
- Balanced Carbohydrate Consumption
While it’s essential to include carbohydrates, choosing wisely and moderating intake is key. Embrace:- Healthy Carbs (e.g., Lentils, Whole Grains): Include these in your diet for a steady release of energy without causing abrupt spikes in blood sugar.
- Healthy Fats
Incorporating healthy fats is essential for a well-rounded diet. Opt for sources like avocados, nuts, and olive oil to promote overall metabolic health. - Apple Cider Vinegar
Some studies suggest that apple cider vinegar may aid in improving insulin sensitivity. Incorporate it into your diet cautiously, considering personal preferences.
In crafting a healthy diet for insulin resistance, focus on balance and variety. Remember, small, sustainable changes can lead to significant improvements in managing and potentially reversing insulin resistance.