Living with diabetes brings forth various challenges, and one of the critical concerns is the development of diabetic ulcers. These wounds, often slow to heal, can pose serious risks if not managed properly. In our blog, we delve into the intricacies of diabetic ulcer treatment, offering insights, strategies, and valuable information to empower individuals in their journey toward healing and overall well-being.
Contents
What Are Diabetic Ulcers?
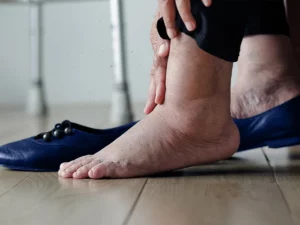 Diabetic ulcers are chronic wounds that commonly develop on the feet of individuals with diabetes due to complications associated with the condition. Diabetes can lead to poor circulation and nerve damage, particularly in the extremities. This makes the feet more susceptible to injuries and slower healing. Diabetic ulcers often emerge as a result of minor cuts, blisters, or pressure points that go unnoticed due to reduced sensation, and the compromised blood flow impedes the natural healing process.
Diabetic ulcers are chronic wounds that commonly develop on the feet of individuals with diabetes due to complications associated with the condition. Diabetes can lead to poor circulation and nerve damage, particularly in the extremities. This makes the feet more susceptible to injuries and slower healing. Diabetic ulcers often emerge as a result of minor cuts, blisters, or pressure points that go unnoticed due to reduced sensation, and the compromised blood flow impedes the natural healing process.
What begins as a seemingly insignificant wound can escalate into a serious ulcer if not promptly addressed. These ulcers pose a significant risk, as they may become infected and, in severe cases, lead to complications such as cellulitis or even limb amputation if left untreated.
The management of diabetic ulcers involves a multi-faceted approach and addressing the underlying factors contributing to delayed healing. Regular monitoring, timely medical intervention, and lifestyle adjustments are crucial components in preventing the escalation of diabetic ulcers.
What Are The Best Diabetic Ulcer Treatment Options?
Effective diabetic ulcer treatment involves a combination of medical interventions, wound care, and lifestyle adjustments to promote healing and prevent complications. Here are some of the best treatment options:
Wound Care and Dressings
Meticulous wound care is the cornerstone of diabetic ulcer treatment. Thoroughly cleaning the ulcer and removing any necrotic tissue (debridement) are crucial steps to create an optimal environment for healing. Appropriate dressings, which may include hydrocolloids or alginate dressings, are applied to protect the wound, absorb excess moisture, and promote tissue regeneration.
Infection Management
Diabetic ulcers are susceptible to infections that can impede the healing process and lead to severe complications. Timely administration of antibiotics, either topically or orally, is often prescribed to treat or prevent infections. Regular monitoring for signs of infection, such as increased redness, swelling, or discharge, is essential for prompt intervention.
Offloading Pressure
Offloading pressure from the affected area is crucial to relieve stress on the ulcer and promote healing. This may involve the use of specialized footwear, orthotic devices, or casting to redistribute pressure and prevent further damage. Offloading strategies are personalized based on the location and severity of the ulcer.
Advanced Therapies
In certain cases, advanced therapies like hyperbaric oxygen therapy (HBOT) may be recommended. HBOT involves exposing the patient to pure oxygen in a pressurized chamber, which enhances oxygen delivery to tissues, reduces inflammation, and promotes wound healing. This therapy is particularly beneficial for chronic, non-healing ulcers.
Growth Factors and Bioengineered Tissues
Topical application of growth factors, such as platelet-derived growth factor (PDGF), and the use of bioengineered tissues can stimulate tissue regeneration. These treatments aim to accelerate the healing process by providing essential growth factors or a scaffold for new tissue formation, especially in cases where conventional approaches may be insufficient.
Managing Blood Sugar Levels
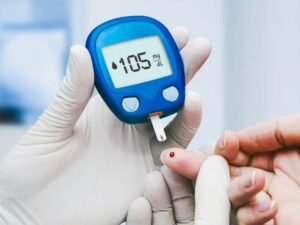 Tight glycemic control is pivotal in diabetic ulcer management. Elevated blood sugar levels impair circulation and compromise the body’s ability to heal. Consistent monitoring and adjustments to insulin or oral medications help maintain blood glucose within the target range, facilitating optimal conditions for wound healing.
Tight glycemic control is pivotal in diabetic ulcer management. Elevated blood sugar levels impair circulation and compromise the body’s ability to heal. Consistent monitoring and adjustments to insulin or oral medications help maintain blood glucose within the target range, facilitating optimal conditions for wound healing.
Nutrition and Hydration
Proper nutrition plays a vital role in supporting the body’s healing mechanisms. A well-balanced diet rich in protein, vitamins, and minerals is essential for tissue repair. Adequate hydration is also crucial as it helps maintain tissue moisture and supports overall bodily functions necessary for healing.
Regular Monitoring
Regular check-ups with healthcare professionals, especially podiatrists and endocrinologists, are essential for monitoring the progress of diabetic ulcers. Through routine examinations, healthcare providers can assess wound healing, and address any emerging issues promptly. And make necessary adjustments to the treatment plan. Consistent monitoring is vital to prevent complications and ensure the effectiveness of the chosen interventions.
It’s important to note that the best treatment plan for diabetic ulcers may vary from person to person. So, healthcare professionals should tailor interventions based on the individual’s specific circumstances and the characteristics of the ulcer. Early intervention and a comprehensive, multidisciplinary approach are key to successful diabetic ulcer management.
Which Ointment Is Best For Diabetic Foot Ulcer?
The choice of ointment for treating diabetic foot ulcers depends on various factors, including the specific characteristics of the ulcer, the presence of infection, and individual patient needs. Commonly used ointments for diabetic foot ulcers may include:
- Silver Sulfadiazine
Silver sulfadiazine is known for its antimicrobial properties and is often used to prevent or treat infections in diabetic foot ulcers. It helps reduce bacterial load and create an environment conducive to wound healing.
- Iodine-Based Ointments
Iodine-based ointments, such as povidone-iodine, have antiseptic properties and can be used to reduce bacterial contamination in diabetic ulcers. These ointments help in preventing and treating infections.
- Honey-Based Ointments
Medical-grade honey, such as manuka honey, has been recognized for its antibacterial and wound-healing properties. It may be used in some cases to promote healing and prevent infection in diabetic foot ulcers.
- Collagenase Ointment
Collagenase ointment contains enzymes that help break down and remove necrotic tissue from the wound. Also, promoting a clean wound bed and facilitating the natural healing process.
- Hydrogel
Hydrogel ointments provide a moist environment for the wound, promoting tissue hydration and facilitating autolytic debridement. They are particularly beneficial for wounds with minimal to no infection.
- Antibiotic Ointments
Topical antibiotic ointments, such as bacitracin or mupirocin, may be prescribed to prevent or treat bacterial infections in diabetic foot ulcers. However, their use should be guided by a healthcare professional to avoid the development of antibiotic resistance.
It’s important to note that while topical ointments can be a component of diabetic foot ulcer care, they are often part of a more comprehensive treatment plan. The choice of ointment should be based on the specific needs of the individual and the characteristics of the diabetic foot ulcer.
How Long Does Diabetic Ulcer Treatment Take To Heal?
 The healing time for diabetic ulcers can vary widely and is influenced by several factors. Diabetic ulcers often require a longer healing time compared to wounds in individuals without diabetes due to impaired circulation, nerve damage, and potential complications.
The healing time for diabetic ulcers can vary widely and is influenced by several factors. Diabetic ulcers often require a longer healing time compared to wounds in individuals without diabetes due to impaired circulation, nerve damage, and potential complications.
On average, small, uncomplicated diabetic ulcers may take several weeks to a few months to heal with appropriate and consistent treatment. However, larger or more severe ulcers, those with infections, or ulcers in individuals with poorly controlled diabetes may take significantly longer to heal.
The key factors that influence the healing time of diabetic ulcers include:
- Early Intervention: Prompt recognition and early intervention play a crucial role in reducing healing time. Timely initiation of appropriate wound care, infection management, and offloading strategies can positively impact the healing process.
- Glycemic Control: Maintaining tight control of blood sugar levels is essential for optimal wound healing. Elevated blood glucose levels can impair circulation and compromise the body’s ability to repair damaged tissues.
- Compliance with Treatment Plan: Adherence to the prescribed treatment plan, including regular wound care, offloading, and other medical interventions, significantly contributes to the effectiveness of the healing process.
- Underlying Health Conditions: The presence of other health conditions. Such as vascular disease or immune system disorders, can influence the healing time of diabetic foot ulcers.
Individuals with diabetic foot ulcers need to work closely with their healthcare team, which may include podiatrists, wound care specialists, and endocrinologists. Regular monitoring, adjustments to the treatment plan as needed, and ongoing communication with healthcare providers are essential. They will help to ensure the best possible outcomes in terms of healing time and prevention of complications.
Conclusion
In conclusion, diabetic ulcers treatment involves a comprehensive approach encompassing timely wound care, infection control, and lifestyle adjustments. By understanding the risks associated with diabetes and prioritizing preventive measures, individuals can significantly reduce the likelihood of developing ulcers. For those already dealing with diabetic foot ulcers, early intervention, adherence to prescribed treatments, and consistent monitoring are crucial for effective healing.
The collaborative efforts of healthcare professionals, including podiatrists and endocrinologists, alongside self-care practices, can empower individuals to navigate the path to recovery. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.