Living with diabetes comes with its own set of challenges, and one common complication that many individuals with diabetes face is cold feet. The sensation of cold feet can be uncomfortable and even painful, affecting one’s daily life. In this comprehensive guide, we’ll delve into the causes of cold feet in diabetes and explore effective treatment methods to bring warmth and comfort back to your feet.
Contents
- 1 Is It Common To Have Cold Feet in Diabetes?
- 2 List of Diabetes Cold Feet Treatment Methods
- 2.1 Blood Sugar Control
- 2.2 Medications
- 2.3 Foot Care
- 2.4 Exercise
- 2.5 Foot Warmers
- 2.6 Elevating Feet
- 2.7 Massage
- 2.8 Warm Foot Baths
- 2.9 Heat Packs
- 2.10 Nutritional Considerations
- 2.11 Consultation with Healthcare Professionals
- 2.12 Compression Stockings
- 2.13 Quit Smoking
- 2.14 Avoid Tight Footwear
- 2.15 Manage Stress
- 3 How To Get Diabetes Cold Feet Treatment?
- 4 Conclusion
Is It Common To Have Cold Feet in Diabetes?
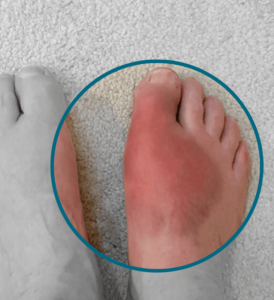
Yes, it is relatively common for individuals with diabetes to experience cold feet. Cold feet can be a symptom of peripheral neuropathy, a common complication of diabetes. Peripheral neuropathy is a condition characterized by nerve damage, often affecting the extremities, such as the feet and legs.
Several factors contribute to cold feet in diabetes:
- Peripheral Neuropathy: Elevated blood sugar levels over time can lead to nerve damage, affecting the nerves that control sensation in the feet. As a result, individuals may experience reduced sensitivity to temperature changes, making the feet feel colder than they are.
- Poor Circulation: Diabetes can also contribute to vascular complications, leading to reduced blood flow to the extremities. Poor circulation can result in cold feet, as the blood may not reach the feet efficiently, affecting both temperature regulation and overall comfort.
- Autonomic Neuropathy: Diabetes can impact the autonomic nerves, which control involuntary bodily functions, including blood vessel dilation. Dysfunction in these nerves can affect the body’s ability to regulate blood flow to the extremities, leading to cold feet.
- Foot Complications: Diabetes can increase the risk of foot problems, such as dry skin, calluses, and foot ulcers. These issues can contribute to discomfort and may make the feet feel colder.
Individuals with diabetes need to pay close attention to their foot health and promptly address any symptoms or complications.
List of Diabetes Cold Feet Treatment Methods
Blood Sugar Control
Diabetes, a chronic condition characterized by elevated blood sugar levels, can lead to various complications, including peripheral neuropathy that contributes to cold feet. Blood sugar control is fundamental in managing diabetes and preventing complications. Regular monitoring of blood glucose levels is essential for understanding how various factors, such as diet, physical activity, and medications, influence blood sugar.
Adherence to prescribed medications, including insulin or oral antidiabetic agents, is crucial to maintain optimal blood sugar levels. A well-balanced diet, rich in fiber, fruits, vegetables, and whole grains, helps regulate blood sugar levels. Controlling blood sugar not only prevents further nerve damage but also plays a key role in managing symptoms like cold feet.
Medications
Nerve pain medications, including gabapentin and pregabalin, are commonly prescribed to manage neuropathic symptoms associated with conditions like diabetic peripheral neuropathy. These medications work by stabilizing abnormal electrical activity in the nerves, providing relief from pain, tingling, and other discomforts.
It’s essential to consult with a healthcare professional to discuss the appropriate medication, dosage, and potential side effects. Regular follow-ups with healthcare providers allow for adjustments in the treatment plan to optimize symptom management.
Foot Care
Daily foot care is crucial for individuals with diabetes to prevent complications such as infections and ulcers. Washing the feet daily with mild soap and warm water helps maintain cleanliness and reduces the risk of infections. Thorough drying, especially between the toes, is essential to prevent fungal growth.
Moisturizing the feet with a gentle lotion or cream prevents dry skin, minimizing the risk of cracks and discomfort. Regular inspection of the feet for cuts, sores, or any abnormalities is vital for early detection and intervention to avoid potential complications.
Exercise
Physical activity plays a pivotal role in diabetes management, particularly in improving circulation and reducing neuropathic symptoms. Aerobic exercises, such as brisk walking, swimming, or cycling, enhance cardiovascular health and contribute to better blood flow to the extremities.
Incorporating resistance training, such as weightlifting or bodyweight exercises, improves muscle strength, supporting overall mobility and reducing the risk of foot-related complications. However, it’s important to consult with a healthcare professional before starting any exercise program to ensure it aligns with individual health needs.
Foot Warmers
Wearing warm socks and utilizing heated insoles can be particularly beneficial for individuals with diabetes experiencing cold feet. Socks made from materials like wool provide insulation and retain heat, offering immediate relief. Meanwhile, heated insoles provide controlled warmth, ensuring comfort throughout the day.
It’s advisable to choose socks with seamless construction to prevent friction and potential skin irritation. Additionally, selecting heated insoles with adjustable temperature settings allows users to customize the warmth based on personal preferences. Regularly inspecting and replacing worn-out socks and insoles is crucial to maintaining their effectiveness in providing warmth and preventing complications.
Elevating Feet
Elevating the feet is a simple yet effective method to improve blood circulation and reduce the sensation of coldness. This practice is especially beneficial for individuals with diabetes who may experience issues with blood flow to the extremities. While sitting or lying down, placing the feet on a comfortable support, such as a cushion or pillow, helps alleviate pressure and promotes venous blood return to the heart.
Regularly incorporating foot elevation into daily routines, particularly during periods of prolonged sitting or resting, can contribute to improved overall comfort.
Massage

Gentle foot massages offer more than just relief from cold feet; they provide an opportunity for self-care and relaxation. Using a moisturizing cream or lotion during massages not only enhances the tactile experience but also contributes to skin hydration. Massaging the feet involves applying gentle pressure to various areas, focusing on the soles, arches, and heels.
This can help stimulate blood circulation, alleviate muscle tension, and reduce neuropathic discomfort. Incorporating foot massages into a nightly routine can serve as a calming ritual, contributing to overall well-being.
Warm Foot Baths
Soaking the feet in warm water, often referred to as a warm foot bath, is a therapeutic practice that brings relief to cold feet. A foot bath not only provides warmth but also helps relax muscles and improve blood circulation. Adding a mild soap or Epsom salts to the water can enhance the soothing effects.
However, it’s crucial to ensure that the water temperature is moderate to avoid burns or adverse reactions, especially for individuals with diabetes who may have reduced sensation. Following the foot bath with thorough drying and moisturizing completes the regimen, promoting skin health and preventing dryness.
Heat Packs
Heat packs, when applied judiciously, can offer targeted warmth to cold feet. They are available in various forms, including electric or microwavable options and adhesive pads. Before application, it’s important to check the temperature to prevent burns. Heat packs can be particularly useful before bedtime to improve sleep quality.
Additionally, incorporating them into a relaxation routine, such as during meditation or while watching TV, provides a dual benefit of warmth and stress relief. However, individuals should exercise caution and follow usage guidelines to prevent any adverse effects.
Nutritional Considerations
Nutritional choices play a significant role in managing diabetes and associated symptoms, including cold feet. Omega-3 fatty acids, found in fatty fish, flaxseeds, and walnuts, possess anti-inflammatory properties that may alleviate neuropathic symptoms. Including these foods in the diet promotes overall cardiovascular health.
Similarly, ensuring an adequate intake of vitamin B12, primarily obtained from animal products like meat, fish, and dairy, supports nerve health. Consulting with a dietitian can help individuals create a well-balanced diet plan that addresses nutritional needs while considering any dietary restrictions.
Consultation with Healthcare Professionals
Regular visits to a podiatrist are essential for individuals with diabetes to proactively manage foot health. Podiatrists specialize in assessing and treating foot-related issues, providing preventive care to avoid complications such as ulcers and infections. An endocrinologist, as a diabetes specialist, collaborates with individuals to optimize overall diabetes management.
This includes adjusting medication regimens, addressing systemic issues, and coordinating with other healthcare professionals to ensure comprehensive care. Open communication with both specialists allows for a holistic approach to diabetes care, reducing the risk of complications.
Compression Stockings
Compression stockings are specialized garments designed to apply gentle pressure to the legs, aiding in blood circulation. They are particularly beneficial for individuals with diabetes who may experience poor circulation, a common contributing factor to cold feet. Proper sizing is essential to ensure optimal compression without causing discomfort.
Healthcare providers can guide individuals on the appropriate compression level and duration of use based on their specific needs. Consistent use of compression stockings can contribute to improved blood flow, reducing symptoms of cold feet and preventing complications associated with poor circulation.
Quit Smoking
Quitting smoking is a crucial step for individuals with diabetes seeking to improve overall health, including blood circulation. Smoking contributes to the narrowing of blood vessels, reducing blood flow to the extremities and exacerbating cold feet symptoms.
Developing a smoking cessation plan involves collaborating with healthcare professionals who can provide support, counseling, and, if necessary, medications to aid in the process. The benefits of quitting extend beyond cold feet, encompassing improvements in cardiovascular and respiratory health.
Avoid Tight Footwear
Choosing appropriate footwear is essential for individuals with diabetes to prevent complications and enhance comfort. Tight shoes can constrict blood flow to the feet, exacerbating cold feet symptoms and increasing the risk of foot-related issues. It’s advisable to select shoes with proper arch support, a roomy toe box, and a comfortable sole. Regularly measuring foot size and replacing worn-out shoes contribute to overall foot health. Additionally, consulting with a podiatrist can provide personalized recommendations for footwear based on individual foot characteristics.
Manage Stress
Chronic stress can amplify neuropathic symptoms, including the sensation of cold feet. Incorporating stress-management techniques into daily life promotes overall well-being. Meditation, deep breathing exercises, yoga, and mindfulness practices are effective methods for reducing stress levels.
Integrating these techniques into a daily routine can have a positive impact on both mental and physical health. Individuals can explore various stress-reduction approaches to identify those that resonate with their preferences and lifestyles.
How To Get Diabetes Cold Feet Treatment?
While it’s important to note that online information can provide general guidance, seeking personalized medical advice from healthcare professionals is crucial for diabetes cold feet treatment. Online platforms can offer resources and information, but the following websites may provide valuable insights into diabetes management and peripheral neuropathy:
- American Diabetes Association (ADA): The ADA offers comprehensive information on diabetes, including tips on managing symptoms and complications. The website provides resources on foot care and neuropathy.
- Diabetes Mantra: Diabetes Mantra is a reputable source of medical information. Their diabetes section covers various aspects of the condition, including complications like neuropathy.
- WebMD: WebMD offers user-friendly information on diabetes and related complications. Their Diabetes Health Center includes articles on peripheral neuropathy and foot care.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): NIDDK, part of the National Institutes of Health (NIH), provides in-depth information on diabetic neuropathies, including tips for prevention and management.
- Diabetes Forecast: Diabetes Forecast is the consumer magazine of the ADA. It provides articles, tips, and resources on various aspects of living with diabetes, including foot care.
- Neuropathy Action Foundation: This organization focuses on peripheral neuropathy and provides resources for individuals dealing with neuropathic symptoms, including those related to diabetes.
Conclusion
Managing cold feet in individuals with diabetes necessitates a holistic approach that combines medical management, lifestyle modifications, and targeted therapies. Consistent monitoring, proper foot care, and collaboration with healthcare professionals are crucial in ensuring the overall well-being of individuals with diabetes experiencing cold feet.
Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.

