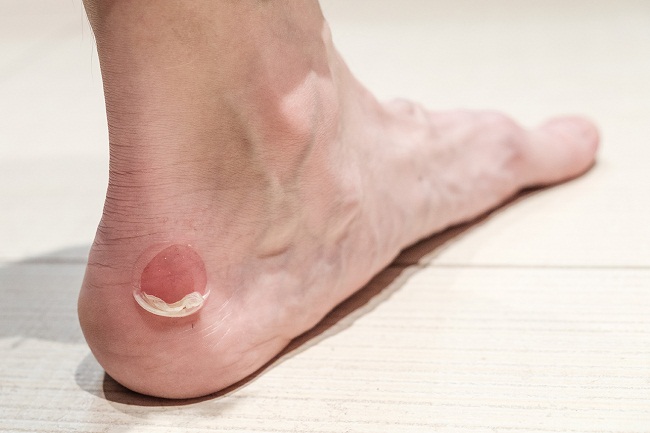
Living with diabetes requires diligent attention to various aspects of health, and one often-overlooked complication is the formation of diabetic blisters. These blisters can be a cause for concern and discomfort, requiring specialized care to promote healing and prevent complications. In this comprehensive guide, we will delve into the world of diabetic blister treatment, offering valuable insights, practical tips, and expert advice to empower individuals with diabetes in managing this aspect of their health.
Contents
Why Do Diabetics Get Blisters?
 Diabetics may be prone to developing blisters due to a combination of factors associated with the disease. Here are some key reasons:
Diabetics may be prone to developing blisters due to a combination of factors associated with the disease. Here are some key reasons:
- Peripheral Neuropathy
Diabetes can lead to peripheral neuropathy, a condition where nerves in the extremities (such as the feet) are damaged. This nerve damage can reduce sensation, making it more likely for individuals with diabetes to overlook minor injuries, including friction or pressure that can cause blisters.
- Poor Circulation
Diabetes can also impact blood circulation, especially to the extremities. Reduced blood flow can hinder the body’s ability to heal wounds and injuries efficiently. And, making diabetics more susceptible to developing blisters and other skin problems.
- Impaired Immune Function
Individuals with diabetes may experience compromised immune function. A weakened immune system can slow down the body’s natural healing processes. Eventually, this makes it harder to fight off infections or prevent the progression of blisters into more severe complications.
- High Blood Sugar Levels
Elevated blood sugar levels over time can affect the skin’s collagen, making it more susceptible to damage and slower to heal. This compromised skin integrity increases the likelihood of developing blisters and other skin-related issues.
- Foot Deformities
Diabetic neuropathy and other complications can lead to changes in the structure of the feet, including deformities and misalignments. These alterations can create areas of increased pressure and friction, contributing to the formation of blisters.
- Footwear and Friction
Ill-fitting footwear or shoes that create excessive friction can contribute to the development of blisters. Diabetics, particularly those with neuropathy, may not feel the discomfort caused by poorly fitting shoes. This allows blisters to form and worsen without immediate awareness.
Individuals with diabetes must prioritize proper foot care, regularly inspect their feet for any signs of injury, and work closely with healthcare professionals to manage blood sugar levels. Early detection and proactive care are essential to minimizing the impact of diabetic blisters.
What Is The Best Diabetic Blister Treatment?
The treatment of diabetic blisters involves a combination of self-care measures, medical intervention when necessary, and preventive strategies. It’s important to note that individual responses to treatment may vary. Thus, consulting with a healthcare professional is essential for personalized guidance. Here are some general approaches to diabetic blister treatment:
Gentle Cleaning
Proper wound care begins with gentle cleaning. Wash the affected area with mild soap and lukewarm water, avoiding hot water that could cause further irritation. Use a soft, clean towel to pat the area dry. This initial step helps to remove debris and bacteria, creating a clean environment for the healing process.
Avoid Popping Blisters
While it may be tempting to pop a blister, especially if it causes discomfort, it’s essential to resist the urge. Diabetic blisters act as a natural barrier, protecting the underlying skin from infection. Puncturing the blister can introduce bacteria, increasing the risk of complications. Instead, focus on protecting the blister and allowing it to heal on its own.
Protective Dressings
Applying a sterile and non-stick dressing is crucial for preventing further friction and protecting the blister from external irritants. Opt for bandages specifically designed for wound care, changing them regularly to maintain cleanliness. This helps create an optimal environment for healing while minimizing the risk of infection.
Topical Antibiotics
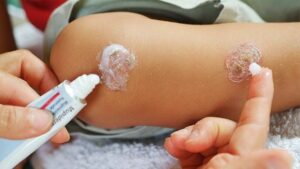 If signs of infection, such as redness, swelling, or increased pain, are present, consult a healthcare professional. They may recommend an over-the-counter or prescription topical antibiotic ointment to prevent or treat infections. This step is crucial in addressing potential complications and supporting the healing process.
If signs of infection, such as redness, swelling, or increased pain, are present, consult a healthcare professional. They may recommend an over-the-counter or prescription topical antibiotic ointment to prevent or treat infections. This step is crucial in addressing potential complications and supporting the healing process.
Offloading Pressure
For blisters on the feet, offloading pressure is key to preventing further irritation. Consider using cushioned insoles or orthotic devices to reduce pressure and friction during walking. Wearing properly fitted and comfortable shoes is equally important in maintaining foot health and avoiding additional trauma to the affected area.
Control Blood Sugar Levels
Maintaining optimal blood glucose levels is a fundamental aspect of diabetic blister treatment. Well-managed diabetes supports overall healing and reduces the risk of complications. Adhering to prescribed medications, adopting a balanced diet, and monitoring blood sugar levels regularly contribute to effective diabetes management.
Regular Monitoring
Keep a vigilant eye on the blister’s progress. If there are any signs of worsening, such as increased redness, swelling, or drainage, seek prompt medical attention. Regular monitoring allows for early detection of potential issues, enabling timely intervention and preventing the development of more severe complications. Stay proactive in observing changes in the blister and the surrounding skin to ensure a swift response to any concerns.
Medical Intervention
In some cases, medical intervention may be necessary, especially if the blister is large, painful, or shows signs of infection. A healthcare professional, such as a doctor or nurse, may need to drain the blister using sterile equipment to relieve pressure and promote faster healing. This procedure should only be performed by qualified individuals to reduce the risk of introducing infections. Seeking medical attention ensures that the blister is properly assessed, and appropriate interventions are implemented based on the specific characteristics of the wound.
Wound Care Clinics
For individuals dealing with persistent diabetic blisters or those with underlying complications, seeking assistance from a wound care clinic or specialist can be beneficial. These clinics often have a multidisciplinary approach to wound management, involving experts such as wound care nurses, podiatrists, and endocrinologists. Specialized wound care professionals can provide advanced treatments, monitor healing progress, and offer tailored advice on preventive measures.
People with diabetes to involve their healthcare team in the management of diabetic blisters. Regular check-ups and communication with healthcare professionals can help address any complications promptly and ensure a comprehensive approach to diabetes care.
How To Prevent Diabetic Blister?
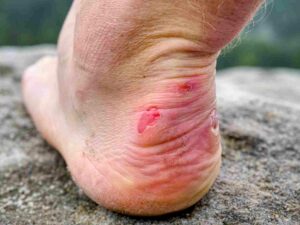 Preventing diabetic blisters involves adopting a proactive approach to foot care and overall diabetes management. Here are some key strategies to help prevent diabetic blisters:
Preventing diabetic blisters involves adopting a proactive approach to foot care and overall diabetes management. Here are some key strategies to help prevent diabetic blisters:
Proper Footwear Selection
Choose shoes that provide adequate support, have a roomy toe box to prevent rubbing, and are made from breathable materials. Avoid shoes with seams or rough edges that could cause friction and irritation. Regularly inspect and replace worn-out shoes.
Moisturize Regularly
Keep the skin on your feet well-moisturized to prevent dryness and cracking, which can increase the risk of blisters. Use a hypoallergenic moisturizer recommended by your healthcare provider and avoid applying it between the toes to prevent excess moisture.
Regular Foot Inspections
Perform daily inspections of your feet to check for any signs of redness, swelling, or areas of increased pressure. Early detection of potential issues allows for prompt intervention and reduces the risk of developing blisters.
Trim Toenails Carefully
Trim your toenails straight across and avoid cutting the corners to prevent ingrown toenails. If you have difficulty trimming your nails, seek assistance from a podiatrist to ensure proper nail care.
Manage Blood Pressure
High blood pressure can contribute to poor circulation and increase the risk of foot complications. Work with your healthcare team to manage and control your blood pressure through lifestyle modifications and prescribed medications.
Stay Active and Maintain a Healthy Weight
Regular physical activity and maintaining a healthy weight contribute to overall health, including improved circulation and reduced pressure on the feet. Consult with your healthcare provider to develop an appropriate exercise routine.
Manage Stress
Chronic stress can impact blood sugar levels and overall health. Practice stress-reducing techniques such as meditation, deep breathing exercises, or engaging in activities you enjoy to promote mental well-being.
Regular Check-Ups
Schedule regular check-ups with your healthcare team, including a podiatrist, to monitor your foot health. Regular professional assessments can help detect potential issues early and guide preventive measures.
Avoid Excessive Heat
Be cautious with hot surfaces, such as heated blankets or water, as diabetes can reduce temperature sensitivity. Use a thermometer to check the water temperature before bathing to avoid burns or blisters.
Wear Seamless Socks
Choose seamless socks made of moisture-wicking materials to minimize friction and reduce the risk of blisters. Seamless socks also decrease the likelihood of irritation on the skin.
By integrating these preventive measures into your daily routine, you can significantly reduce the risk of developing diabetic blisters and promote overall foot health. Regular communication with your healthcare team is essential to tailor these strategies to your individual needs and circumstances.
Conclusion
In conclusion, diabetic blister treatment requires attentive care, proactive steps, and a commitment to overall well-being. By understanding the causes, signs, and effective treatment options outlined in this guide, individuals with diabetes can take control of their foot health. Remember to prioritize gentle cleaning, avoid popping blisters, and seek medical attention when needed. Embrace preventive measures like proper footwear, regular foot inspections, and maintaining optimal blood sugar levels to minimize the risk of blisters.
Ultimately, a holistic approach, including lifestyle adjustments and regular check-ups, empowers individuals to navigate the challenges of diabetic blister care with confidence, promoting faster healing and reducing the likelihood of complications. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.