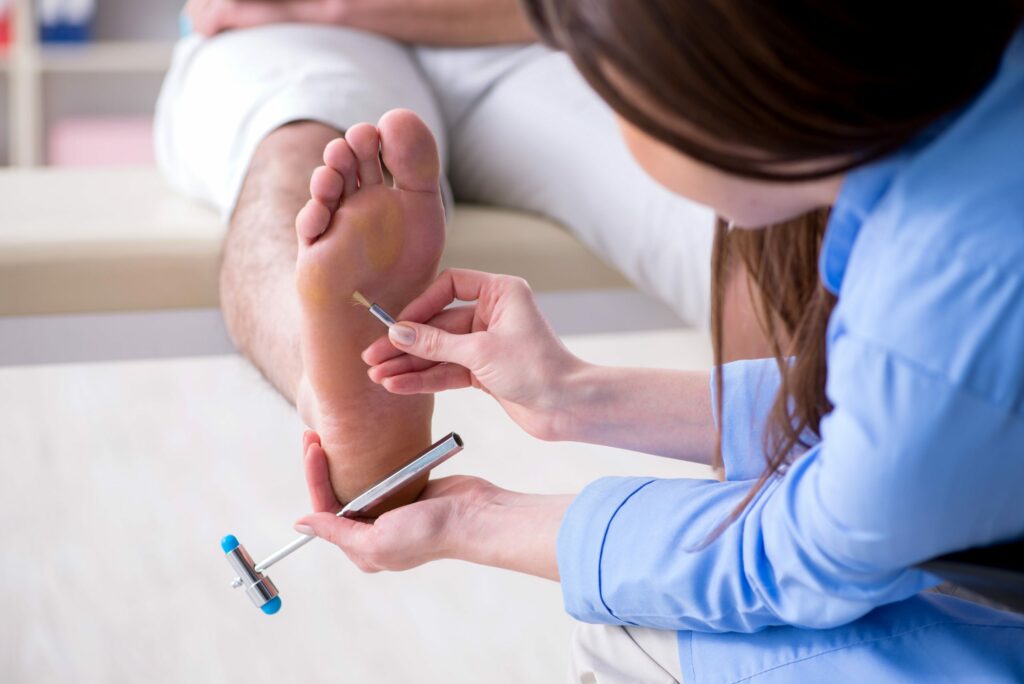
Diabetic nerve pain, also known as diabetic neuropathy, is a common and often debilitating complication of diabetes. It arises when prolonged high blood sugar levels damage the nerves throughout the body, leading to symptoms such as tingling, numbness, burning sensations, and pain. Managing diabetic nerve pain is crucial for improving the quality of life for individuals with diabetes. One key aspect of this management is the use of medications specifically designed to alleviate the symptoms and slow down the progression of neuropathy. In this blog post, we will explore the various medication for diabetic nerve pain, their mechanisms of action, potential side effects, and how they fit into an overall treatment plan.
Contents
Is Nerve Pain a Common Sign in Diabetes?

Yes, nerve pain is a common sign of diabetes, and it is often associated with a condition known as diabetic neuropathy. Diabetic neuropathy is a type of nerve damage that can occur as a complication of diabetes, particularly when blood sugar levels are consistently high over an extended period. The condition affects nerves throughout the body, leading to various symptoms, including pain, tingling, numbness, and weakness.
There are several types of diabetic neuropathy, and each can affect different nerves in the body:
- Peripheral Neuropathy: This is the most common form of diabetic neuropathy and typically affects the nerves in the feet and legs. Symptoms may include tingling, burning, numbness, and pain. Peripheral neuropathy can also lead to difficulties in balance and coordination.
- Autonomic Neuropathy: This type of neuropathy affects the nerves that control involuntary bodily functions such as digestion, heart rate, and blood pressure. It can lead to symptoms such as gastrointestinal issues, urinary problems, and changes in heart rate.
- Proximal Neuropathy: This type of neuropathy affects the nerves in the thighs, hips, or buttocks, causing weakness and pain. It can also lead to difficulties in leg movement.
- Focal Neuropathy: Focal neuropathy results in sudden, intense pain in specific nerves or groups of nerves. It can affect the eyes, facial muscles, or other parts of the body.
The pain associated with diabetic neuropathy is often described as burning, stabbing, or shooting. It can be constant or intermittent and may worsen at night. Additionally, individuals with diabetic neuropathy may experience heightened sensitivity to touch or temperature changes.
List of Diabetic Nerve Pain Medication
There are various medications used to manage diabetic nerve pain, also known as diabetic neuropathy. It’s important to note that the choice of medication depends on factors such as the type and severity of symptoms, individual response, and potential side effects. Here is a list of common medications prescribed for diabetic nerve pain:
Gabapentin
Gabapentin is an anticonvulsant medication that is commonly prescribed for diabetic nerve pain, also known as diabetic neuropathy. While originally developed to treat seizures, its effectiveness in managing neuropathic pain has led to its widespread use for conditions like diabetic neuropathy.
Gabapentin works by stabilizing electrical activity in the brain and affecting the way nerves send signals. It is thought to modulate the release of certain neurotransmitters involved in transmitting pain signals. This modulation helps reduce the perception of pain and provides relief for individuals experiencing diabetic nerve pain.
Pregabalin
Pregabalin is another anticonvulsant medication that is effective in treating diabetic nerve pain. Similar to gabapentin, pregabalin works by binding to calcium channels in the central nervous system, reducing the release of neurotransmitters involved in pain signaling. This modulation of neurotransmitter release helps alleviate neuropathic pain.
Pregabalin is known for its ability to provide relief from the stabbing, burning, or shooting pains associated with diabetic neuropathy. It is often prescribed as part of a comprehensive treatment plan for managing diabetic nerve pain.
Duloxetine
Duloxetine is a selective serotonin and norepinephrine reuptake inhibitor (SSNRI) that is approved for the treatment of diabetic neuropathy. As an antidepressant, duloxetine is believed to work by increasing the levels of serotonin and norepinephrine in the brain. However, its pain-relieving properties extend beyond its antidepressant effects.
Duloxetine is thought to modulate pain signals in the central nervous system, providing relief for individuals with diabetic nerve pain. This dual mechanism of action makes it a valuable medication for managing both the emotional and physical aspects of diabetic neuropathy.
Amitriptyline
Amitriptyline is a tricyclic antidepressant (TCA) that is sometimes prescribed for diabetic nerve pain. TCAs like amitriptyline alter the levels of certain neurotransmitters in the brain, including serotonin and norepinephrine. By doing so, these medications can influence the way the central nervous system processes pain signals.
Amitriptyline is known for its analgesic properties and is often used to alleviate the neuropathic pain associated with diabetic neuropathy. It is important to note that TCAs may have side effects, and their use for diabetic nerve pain is carefully monitored by healthcare providers.
Capsaicin Cream
Capsaicin cream is a topical medication derived from chili peppers. It is applied directly to the skin over the painful areas, providing relief for localized diabetic nerve pain. Capsaicin works by depleting a neurotransmitter called substance P, which plays a role in transmitting pain signals. The depletion of substance P leads to a reduction in pain sensations.
While capsaicin cream can be effective, it may cause a burning sensation initially, and regular use is often necessary to maintain its pain-relieving effects.
Nortriptyline
Nortriptyline is a tricyclic antidepressant (TCA) similar to amitriptyline. It affects the levels of neurotransmitters in the brain, including serotonin and norepinephrine. By influencing these neurotransmitters, nortriptyline can modulate pain signals and provide relief for diabetic nerve pain. It is often prescribed in cases where TCAs are considered suitable for managing neuropathic pain.
Tramadol
Tramadol is an opioid analgesic that is sometimes prescribed for moderate to severe diabetic nerve pain. It works by binding to opioid receptors in the brain and spinal cord, inhibiting the transmission of pain signals. Tramadol is considered when other non-opioid medications have not provided sufficient pain relief. However, its use is closely monitored due to the potential for dependence and side effects.
Oxycodone
Oxycodone is another opioid medication used for the management of severe diabetic nerve pain. Like tramadol, it binds to opioid receptors, blocking the perception of pain. Oxycodone is generally reserved for cases where other medications have not been effective, and its use requires careful monitoring due to the risk of dependence and respiratory depression.
Topiramate
Topiramate is an anticonvulsant that is sometimes prescribed for diabetic neuropathy. It works by modulating the activity of neurotransmitters in the brain, including glutamate. By stabilizing electrical activity in the central nervous system, topiramate can help reduce the intensity of neuropathic pain. It is often used as an alternative or adjunct to other anticonvulsants in the management of diabetic nerve pain.
Alpha-Lipoic Acid
While not a traditional medication, alpha-lipoic acid is a supplement that has shown promise in managing diabetic neuropathy. It is an antioxidant that may help improve nerve function and reduce oxidative stress. Alpha-lipoic acid is believed to have neuroprotective effects, making it a complementary approach in the overall management of diabetic nerve pain.
How To Take Diabetic Nerve Pain Medication?
Taking diabetic nerve pain medication involves careful adherence to the prescribed dosage and guidelines provided by healthcare professionals. Here’s a concise set of points on how to take diabetic nerve pain medication:
Follow Prescribed Dosage:
- Take the medication exactly as prescribed by your healthcare provider.
- Do not self-adjust the dosage without consulting your healthcare provider.
Consistent Timing:
- Take the medication at the same time each day to maintain a consistent level in your bloodstream.
- Set reminders or integrate medication into daily routines to enhance adherence.
With or Without Food:
- Follow specific instructions regarding whether to take the medication with or without food.
- Some medications are more effective when taken with a meal, while others may require an empty stomach.
Avoid Alcohol and Grapefruit:
- Limit or avoid alcohol consumption as it may interact with certain medications.
- Check with your healthcare provider about any restrictions related to grapefruit, as it can interfere with some medications.
Monitor for Side Effects:
- Be vigilant for potential side effects such as dizziness, drowsiness, or gastrointestinal issues.
- Report any unexpected or severe side effects to your healthcare provider promptly.
Regular Follow-Up Appointments:
- Attend scheduled follow-up appointments with your healthcare provider to assess the medication’s effectiveness and adjust the treatment plan if necessary.
Do Not Skip Doses:
- Take the medication consistently, even if you feel better.
- Skipping doses may compromise the effectiveness of the treatment.
Storage and Expiry:
- Store medications as directed, paying attention to temperature and humidity requirements.
- Discard any expired medication and obtain a new prescription if needed.
Communicate Changes:
- Inform your healthcare provider of any changes in your overall health, including new symptoms or the development of other medical conditions.
- Report any changes in your diabetes management, such as alterations in blood sugar levels.
Be Aware of Interactions:
- Inform your healthcare provider about all medications, supplements, or herbal remedies you are taking to avoid potential interactions.
- Follow advice on spacing medications if certain combinations are not recommended to be taken simultaneously.
Seek Emergency Help if Necessary:
- In case of severe side effects or allergic reactions, seek emergency medical attention.
- Be aware of the signs of a medical emergency and have a plan in place.
Considerations for Diabetic Nerve Pain Medication

When considering diabetic nerve pain medication, several important factors should be taken into account to ensure effective and safe management of symptoms. Here are key considerations:
Individualized Treatment Plans:
- Medication choices should be tailored to the individual’s specific symptoms, medical history, and overall health.
- The severity of neuropathy, the presence of other health conditions, and potential drug interactions all influence the selection of appropriate medications.
Consultation with Healthcare Provider:
- Always consult with a healthcare provider before starting any new medication for diabetic nerve pain.
- Discuss your complete medical history, including allergies and existing medications, to avoid potential interactions.
Comprehensive Assessment:
- A thorough evaluation of the nature and intensity of diabetic nerve pain is essential for choosing the most suitable medication.
- Understanding the impact of pain on daily activities and quality of life helps guide treatment decisions.
Monitoring Blood Sugar Levels:
- Regular monitoring of blood sugar levels is crucial, as uncontrolled diabetes can exacerbate neuropathy.
- Medication adjustments may be necessary based on changes in blood sugar levels and overall diabetes management.
Potential Side Effects:
- Be aware of potential side effects associated with each medication.
- Communicate any side effects promptly to the healthcare provider to address concerns and explore alternative options if needed.
Risk of Dependence and Abuse:
- Opioid medications, such as tramadol and oxycodone, carry a risk of dependence and abuse.
- Healthcare providers must carefully weigh the benefits and risks before prescribing opioids, considering the potential for addiction and the availability of alternative treatments.
Gradual Titration:
- Some medications, particularly anticonvulsants and antidepressants, may require a gradual titration to achieve an optimal therapeutic effect.
- Follow the prescribed dosage schedule and titration plan provided by the healthcare provider.
Compliance and Adherence:
- Patient adherence to the prescribed medication regimen is crucial for effective management.
- Education on the importance of consistent dosing and regular follow-up appointments helps promote adherence.
Conclusion
Diabetic nerve pain can significantly impact the quality of life for individuals with diabetes, but with proper management, the symptoms can be alleviated. Medications play a crucial role in this management, offering relief from pain and improving overall well-being. However, a personalized approach that considers individual health factors, lifestyle, and potential side effects is essential for optimal outcomes. By working closely with healthcare providers and adopting a holistic approach to care, individuals with diabetic nerve pain can take meaningful steps towards better health and reduced discomfort.
Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.