Among the many complications of diabetes, one of the most challenging is the development of wounds, particularly on the feet and lower limbs. These wounds are not only difficult to heal but also pose a significant risk of infection, which can lead to serious health consequences. In this guide, we’ll explore the best practices used in diabetic wound treatment. We will provide valuable insights into the causes and about the several treatment options and preventive measures.
Contents
What Causes Diabetic Wounds?
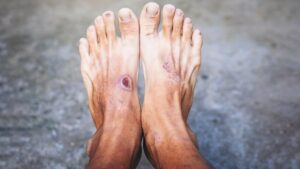 Diabetic wounds, particularly those affecting the lower extremities like the feet, are a common and serious complication of diabetes. The causes of these wounds are multifaceted, often involving a combination of factors associated with diabetes:
Diabetic wounds, particularly those affecting the lower extremities like the feet, are a common and serious complication of diabetes. The causes of these wounds are multifaceted, often involving a combination of factors associated with diabetes:
- Poor Blood Circulation: Diabetes can lead to poor blood flow, especially in the extremities. Reduced circulation means less oxygen and fewer nutrients reach the skin and underlying tissues, impairing the body’s ability to heal wounds effectively.
- Nerve Damage (Neuropathy): High blood sugar levels over time can damage the nerves, particularly in the feet and legs. This condition, known as diabetic neuropathy, results in reduced sensation. Consequently, individuals may not feel minor cuts, blisters, or pressure sores that can develop into more serious wounds.
- Immune System Dysfunction: Diabetes can weaken the immune system, making it less effective in fighting off infections. Even small wounds can quickly become serious if the body cannot effectively combat bacteria.
- High Blood Sugar Levels: Elevated glucose levels in the blood can contribute to the slow healing of wounds. High sugar levels can interfere with the body’s natural healing processes and increase the risk of infection.
- Pressure and Irritation: Due to the loss of sensation and possible deformities (like Charcot foot), diabetic patients might not adjust their posture or footwear to relieve pressure. Continuous pressure or irritation on specific parts of the foot can lead to skin breakdown, resulting in ulcers.
- Inadequate Footwear: Wearing shoes that don’t fit well or that offer poor support can cause pressure points or rub against the skin, leading to blisters, sores, and ulcers.
Understanding these causes is crucial in the management and prevention of diabetic wounds. Regular monitoring and seeking prompt medical attention for any injuries or abnormalities are key strategies in preventing these wounds from developing or worsening.
How Do You Clean A Diabetic Foot Wound?
Cleaning a diabetic foot wound is a critical step in preventing infection and promoting healing. It’s important to follow proper wound care procedures to minimize complications. Here’s a general guideline on how to clean a diabetic foot wound:
1. Wash Your Hands
Before touching the wound, make sure to wash your hands thoroughly with soap and water to avoid introducing bacteria to the wound site.
2. Prepare the Area
Remove any bandages or dressings. If the wound is covered by clothing, gently expose the area. Ensure you’re in a clean environment to reduce the risk of contamination.
3. Gentle Cleaning
Rinse the wound gently with lukewarm water to remove any loose debris or dirt. Avoid using high-pressure water which can damage the tissue.
Use a mild soap or a cleanser recommended by your healthcare provider to clean the skin around the wound. Do not apply soap directly to the wound as it can irritate it.
Avoid using hydrogen peroxide, iodine, or alcohol on the wound. These substances can damage the tissue and delay healing.
4. Pat Dry
After cleaning, gently pat the area dry with a clean, soft towel. Be careful not to rub the wound, as this can cause further irritation or damage.
5. Apply an Antibiotic Ointment
If advised by your healthcare provider, apply a thin layer of an antibiotic ointment to prevent infection.
6. Redress the Wound
Cover the wound with a sterile dressing. Use a bandage that is appropriate for the size and location of the wound. The dressing should be secure but not too tight, as it can restrict blood flow.
7. Monitor the Wound
Regularly check the wound for signs of infection, such as increased redness, swelling, warmth, foul odor, or discharge. Also, monitor for increased pain or fever.
8. Change Dressings Regularly
Follow your healthcare provider’s instructions on how often to change the dressing. Generally, a wound dressing should be changed daily or more often if it becomes wet or dirty.
Remember, each individual’s situation can be unique, especially when managing diabetes and its complications. Therefore, it’s always best to follow the specific instructions given by your healthcare provider or a wound care specialist.
What Is The Best Medicine For Diabetic Wound Treatment?
 It’s essential to have diabetic wounds assessed by a healthcare provider, as treatment should be tailored to individual needs. However, some common types of treatments and medications used in managing diabetic wounds include:
It’s essential to have diabetic wounds assessed by a healthcare provider, as treatment should be tailored to individual needs. However, some common types of treatments and medications used in managing diabetic wounds include:
Antibiotics
In diabetic wounds, especially those with signs of infection like redness, swelling, or discharge, antibiotics are crucial. The choice of antibiotic depends on the type of bacteria causing the infection and its severity. Topical antibiotics are applied directly to the wound and are often used for mild infections, whereas oral or intravenous antibiotics may be required for more severe or deep infections. Patients need to complete the full course of antibiotics to ensure the infection is fully eradicated.
Antiseptics
These are used to clean wounds and prevent infection. Saline solution is commonly used for gentle wound cleaning because it’s isotonic and less irritating to the skin. Iodine-based solutions are effective against a wide range of microorganisms, but they should be used cautiously as they can impede wound healing if used excessively.
Topical Wound Care Products
These products create a conducive environment for wound healing. For example, hydrogel dressings keep the wound moist, which can accelerate healing. Alginate dressings, derived from seaweed, are highly absorbent and suitable for wounds with significant exudate. Some dressings contain silver. It has antimicrobial properties, helping to reduce infection risk.
Pain Management
Pain associated with diabetic wounds can be significant. Over-the-counter pain relievers like acetaminophen (Tylenol) are often recommended because they are less likely to cause stomach upset or bleeding compared to NSAIDs like ibuprofen. However, all medications should be used under medical supervision, especially in individuals with diabetes who may have other health concerns.
Advanced Therapies
For wounds that do not respond to standard treatments, advanced options may be considered. Hyperbaric oxygen therapy involves breathing pure oxygen in a pressurized room. This can enhance oxygen delivery to the wound, promoting healing. Negative pressure wound therapy (NPWT) uses a vacuum pump to create a negative pressure environment around the wound, helping to reduce swelling, remove excess fluid, and promote tissue growth.
Blood Sugar Control Medications
Good glycemic control is essential in wound healing. Poorly controlled blood sugar can impair the immune system and reduce blood flow, slowing down the healing process. Medications that effectively manage blood glucose levels, along with dietary control and regular monitoring, play a significant role in the overall management of diabetic wounds.
Debridement Medications
These are used to help remove dead or infected tissue from the wound, a process essential for healing. Chemical debridement uses special enzymes or other compounds to break down dead tissue. Surgical debridement might be necessary for more severe cases where dead tissue must be physically removed to allow healthy tissue to heal.
Overall, each of these diabetic wound treatment modalities plays a vital role. The choice of treatment depends on the wound’s characteristics and the individual’s overall health status. However, regular assessment by healthcare professionals is important for effective wound management in diabetic patients.
How Long Do Diabetic Wounds Take To Heal?
 The healing time for diabetic wounds varies significantly depending on several factors. Due to the complexities associated with diabetes, these wounds generally take longer to heal compared to those in non-diabetic individuals. The duration can range from weeks to months, and in some cases, they may not heal entirely without intensive treatment. Here are key factors that influence the healing time:
The healing time for diabetic wounds varies significantly depending on several factors. Due to the complexities associated with diabetes, these wounds generally take longer to heal compared to those in non-diabetic individuals. The duration can range from weeks to months, and in some cases, they may not heal entirely without intensive treatment. Here are key factors that influence the healing time:
- Blood Sugar Control: Elevated blood sugar levels can impair the body’s natural healing processes. Tight glucose control is essential for promoting wound healing. Poorly controlled diabetes can lead to prolonged wound healing times.
- Wound Severity and Location: Deeper wounds or those located in areas with poor circulation (like the feet) tend to heal more slowly. Minor surface wounds may heal more quickly if properly cared for.
- Presence of Infection: Infections can significantly delay wound healing. Infected wounds often require antibiotic treatment and more intensive care, which can extend the healing process.
- Individual Health and Lifestyle Factors: Overall health, nutrition, smoking status, and lifestyle choices play significant roles in wound healing. Nutritional deficiencies, smoking, and poor health habits can impede the healing process.
- Treatment and Care: The efficacy of the treatment plan, including proper wound cleaning, appropriate dressings, off-loading (reducing pressure on the wound), and following medical advice, greatly affects the healing time.
Given these variables, it’s difficult to specify an exact timeline for a diabetic wound to heal. Hence, individuals with diabetes need to seek prompt medical attention for any wounds, especially on the feet, and follow the treatment plan prescribed by their healthcare provider.
Conclusion
In conclusion, effectively managing diabetic wounds involves understanding their causes, ensuring prompt and proper care, and adopting a multidisciplinary approach. Good blood sugar control, regular foot inspections, and immediate attention to any injuries are fundamental. Overall, choosing the right diabetic wound treatment, whether it’s antibiotics, specialized dressings, or advanced therapies, depends on each wound’s unique characteristics.
Thus, patients must also focus on lifestyle factors like nutrition and smoking cessation to aid healing. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.