Proximal neuropathy, a condition characterized by nerve damage in the upper part of the body, can be a challenging and often painful experience for those affected. This blog aims to shed light on this lesser-known type of neuropathy, focusing on its causes and the proximal neuropathy treatment options. By understanding more about proximal neuropathy, those who suffer from it can find effective ways to manage their condition and improve their quality of life.
Contents
What Causes Proximal Neuropathy Treatment?
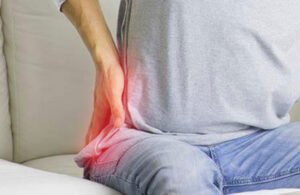 The term “Proximal Neuropathy” refers to a type of nerve damage that affects the upper part of the body, particularly in the hip, buttock, or thigh areas. It’s important to clarify that proximal neuropathy itself is a condition, not a treatment. The causes of proximal neuropathy are varied and can include:
The term “Proximal Neuropathy” refers to a type of nerve damage that affects the upper part of the body, particularly in the hip, buttock, or thigh areas. It’s important to clarify that proximal neuropathy itself is a condition, not a treatment. The causes of proximal neuropathy are varied and can include:
- Diabetes: This is one of the most common causes of proximal neuropathy, often referred to as diabetic amyotrophy. High blood sugar levels over time can damage the nerves, leading to neuropathy.
- Autoimmune Diseases: Conditions like lupus, rheumatoid arthritis, or vasculitis can lead to inflammation of nerves, causing proximal neuropathy.
- Infections: Certain infections, especially viral ones like shingles (herpes zoster), can cause nerve damage leading to neuropathy.
- Neuromuscular Diseases: Diseases such as amyotrophic lateral sclerosis (ALS) and multiple sclerosis (MS) can affect the nerves in the proximal regions of the body.
- Injury or Trauma: Physical trauma or injury to the nerves, due to accidents, falls, or surgeries, can lead to proximal neuropathy.
- Chemotherapy and Other Medications: Some drugs, particularly those used in chemotherapy, can damage nerves and lead to neuropathy.
- Nutritional Deficiencies: Deficiencies in certain vitamins, such as B vitamins (B1, B6, B12), which are crucial for nerve health, can result in nerve damage.
- Alcohol Abuse: Chronic alcoholism can lead to nutrient deficiencies and direct nerve damage, resulting in neuropathy.
- Idiopathic: In some cases, the cause of proximal neuropathy remains unknown, and this is referred to as idiopathic proximal neuropathy.
The treatment for proximal neuropathy typically focuses on managing the underlying cause, if known, and alleviating symptoms. Individuals with symptoms of proximal neuropathy must consult healthcare professionals for an accurate diagnosis and appropriate treatment plan.
What Are The Effective Proximal Neuropathy Treatment?
Effective proximal neuropathy treatment typically focuses on managing symptoms, slowing the progression of the condition, and maintaining quality of life. The specific approach can vary depending on the underlying cause of the neuropathy and the severity of symptoms. Here are some common treatments:
Medications
- Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help manage mild to moderate pain. For more severe pain, doctors may prescribe stronger painkillers. Tricyclic antidepressants, such as amitriptyline, and serotonin-norepinephrine reuptake inhibitors (SNRIs) like duloxetine, are often used for chronic neuropathic pain even though they are primarily designed for depression.
- Anticonvulsants: Medications like gabapentin (Neurontin) and pregabalin (Lyrica) are originally designed for epilepsy but are effective in controlling neuropathic pain. They work by stabilizing electrical activity in the nerves and preventing abnormal nerve transmission.
- Topical Treatments: These are applied directly to the skin and can provide localized pain relief. Capsaicin cream, derived from chili peppers, can desensitize pain receptors over time, while lidocaine patches can numb the affected area.
Physical Therapy

- A physical therapist can develop a tailored exercise program to strengthen muscles weakened by neuropathy, improve balance, and increase flexibility. This can help reduce pain and improve mobility.
- Techniques like transcutaneous electrical nerve stimulation (TENS) may be used. This involves applying a gentle electric current to the skin to disrupt pain signals.
- For some patients, aquatic therapy in a pool can be beneficial, as the buoyancy of water reduces stress on muscles and joints while providing resistance to exercise.
Lifestyle Modifications
- Exercise, such as walking, swimming, or cycling, can improve blood flow to the nerves, potentially reducing symptoms. It’s also crucial for controlling blood sugar levels in diabetic patients.
- Maintaining a healthy weight is important to reduce the burden on nerves and prevent additional nerve damage.
- Smoking cessation is vital since smoking can affect circulation, worsening neuropathic symptoms. Limiting alcohol is also recommended as excessive alcohol can worsen nerve damage.
Dietary Changes
- A diet rich in fruits, vegetables, whole grains, and lean protein can support nerve health. Avoiding foods high in sugars and saturated fats is also beneficial.
- Vitamins B1, B6, B12, and E are particularly important for nerve health. In some cases, supplementation may be necessary, especially for patients with dietary deficiencies.
- It’s also important to stay hydrated, as dehydration can exacerbate symptoms of neuropathy.
Control of Underlying Conditions
- For those with diabetic neuropathy, controlling blood sugar levels is crucial. This might involve medication, dietary changes, and regular blood sugar monitoring.
- Autoimmune conditions, such as lupus or rheumatoid arthritis, can cause neuropathy. Managing these conditions with appropriate medications can help reduce symptoms.
- Thyroid disorders can also contribute to neuropathic pain. Proper treatment of hypothyroidism or hyperthyroidism can alleviate some symptoms of neuropathy.
Alternative Therapies

- Acupuncture: This traditional Chinese medicine technique involves inserting thin needles into specific points on the body. It’s thought to stimulate nerves, muscles, and connective tissue, which can boost natural painkillers and increase blood flow.
- Biofeedback: This technique uses electronic monitoring to teach patients to control certain bodily functions, such as muscle tension or heart rate, which can help manage pain.
- Meditation and Mindfulness: These practices can help individuals manage the stress and anxiety that often accompany chronic pain. Mindfulness-based stress reduction (MBSR) is a program that combines meditation and yoga, and it has been found effective for pain management.
- Herbal Remedies and Supplements: Certain supplements, such as alpha-lipoic acid, have been studied for their potential to improve neuropathic symptoms. However, it’s crucial to discuss with a healthcare provider before starting any supplement, as they can interact with medications.
Assistive Devices
- Braces and Orthotics: These can provide support, reduce pain, and prevent further injury. For example, a hand brace can stabilize the wrist and reduce pain caused by movements that irritate the nerve.
- Mobility Aids: Canes, walkers, or wheelchairs might be necessary for individuals with severe muscle weakness or balance problems. These aids can help maintain independence and prevent falls.
Surgical Intervention
- Surgery may be an option in cases where neuropathy is caused by physical nerve compression, such as in carpal tunnel syndrome or other entrapment neuropathies. The procedure typically involves relieving pressure on the affected nerve.
- For more severe cases, nerve decompression surgery might be considered. However, the effectiveness of surgery depends on various factors, including the cause of neuropathy and overall health.
Psychological Support
- Counseling: Speaking with a mental health professional can help individuals cope with the emotional and psychological effects of living with chronic pain. Techniques like cognitive-behavioral therapy (CBT) can be particularly effective.
- Support Groups: Joining a support group for people with neuropathy can provide a sense of community and mutual understanding. Sharing experiences and tips can be very empowering.
- Stress Management Techniques: Practices like guided imagery, deep breathing exercises, and progressive muscle relaxation can help manage the stress that often exacerbates pain symptoms.
Individuals with proximal neuropathy need to work closely with their healthcare providers to develop a personalized treatment plan that addresses their specific needs and symptoms. Regular follow-up is also important to monitor the condition and adjust treatments as necessary.
How Long Does Proximal Neuropathy Last?
 The duration of proximal neuropathy varies widely depending on its underlying cause and the effectiveness of the treatment approach. In cases where proximal neuropathy is caused by acute conditions, such as a specific injury or a treatable illness, the symptoms may resolve completely with proper treatment. The recovery time in these instances can range from a few weeks to several months, depending largely on the extent of the nerve damage and the body’s response to treatment.
The duration of proximal neuropathy varies widely depending on its underlying cause and the effectiveness of the treatment approach. In cases where proximal neuropathy is caused by acute conditions, such as a specific injury or a treatable illness, the symptoms may resolve completely with proper treatment. The recovery time in these instances can range from a few weeks to several months, depending largely on the extent of the nerve damage and the body’s response to treatment.
However, in chronic conditions like diabetes or autoimmune diseases, proximal neuropathy can be a long-term or even lifelong condition. For such chronic cases, the focus generally shifts to managing symptoms and preventing further nerve damage, rather than complete recovery. The progression of the neuropathy in these scenarios can sometimes be slowed or halted with effective management, but the nerve damage that has already occurred may be irreversible.
Conclusion
In conclusion, proximal neuropathy treatment involves a multifaceted approach that includes medications for pain and nerve health, physical therapy to strengthen and maintain mobility, lifestyle changes for overall well-being, dietary adjustments to support nerve function, and managing any underlying health conditions. While the duration and severity of proximal neuropathy can vary greatly depending on its cause and treatment, adopting a comprehensive management plan can improve quality of life.
Individuals with proximal neuropathy need to work closely with their healthcare providers, stay informed about their condition, and make lifestyle choices that support their overall health and well-being. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.

