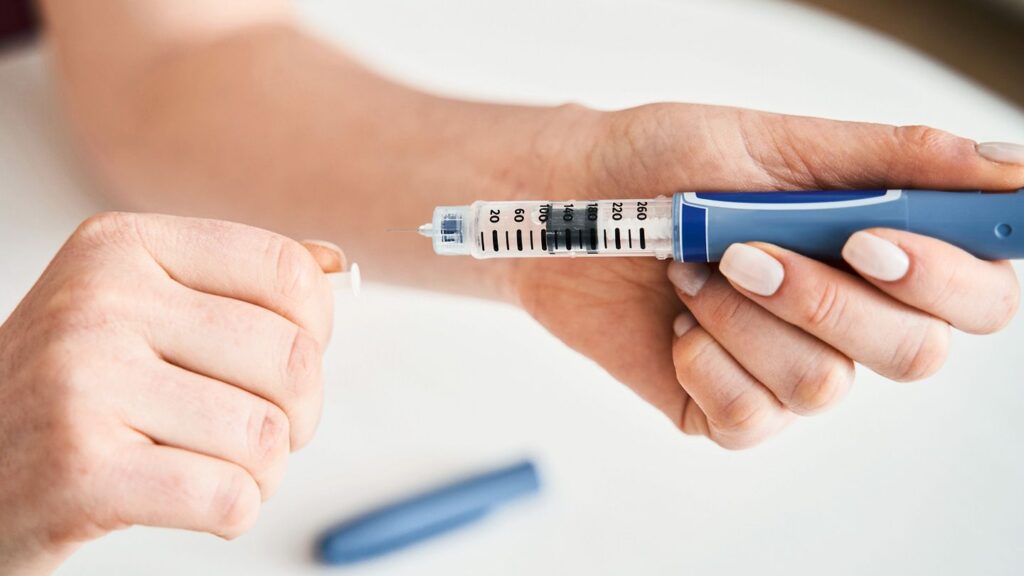
Type 1 diabetes, a chronic condition traditionally managed through regular insulin injections, presents unique challenges and demands constant vigilance from those affected. While insulin therapy remains the cornerstone of treatment, recent advancements in medicine and technology have opened new avenues for managing this condition. This blog aims to explore the strategies for diabetes type 1 treatments without insulin that offer hope and improved quality of life.
Contents
Is It Possible To Manage Type 1 Diabetes Without Insulin?
 Managing Type 1 diabetes without insulin is not currently possible. Type 1 diabetes is an autoimmune condition in which the body’s immune system attacks and destroys the insulin-producing beta cells in the pancreas. As a result, the body is unable to produce insulin, a hormone crucial for regulating blood sugar levels.
Managing Type 1 diabetes without insulin is not currently possible. Type 1 diabetes is an autoimmune condition in which the body’s immune system attacks and destroys the insulin-producing beta cells in the pancreas. As a result, the body is unable to produce insulin, a hormone crucial for regulating blood sugar levels.
Insulin therapy is essential for people with Type 1 diabetes because it replaces the insulin that the body cannot produce. Without insulin, individuals with Type 1 diabetes would experience dangerously high blood sugar levels. Ultimately, leading to serious and potentially life-threatening complications such as diabetic ketoacidosis.
While there is ongoing research into alternative treatments and potential cures for Type 1 diabetes, none have yet been developed that can fully replace the need for insulin therapy. The mainstay of treatment for Type 1 diabetes remains lifelong insulin administration, typically through injections or an insulin pump.
What Happens If a Type 1 Diabetic Eats Without Insulin?
If a person with Type 1 diabetes eats without taking insulin, several significant physiological effects can occur. When a person eats, their blood sugar levels rise, and insulin is needed to help transport this glucose into cells.
Without insulin, this process is disrupted, leading to a series of events:
- High Blood Sugar (Hyperglycemia): When a Type 1 diabetic eats without taking insulin, glucose cannot enter the cells and instead accumulates in the bloodstream, causing high blood sugar levels. This can lead to symptoms such as increased thirst, frequent urination, fatigue, and blurred vision in the short term.
- Cell Starvation: Despite the high levels of glucose in the blood, without insulin, the body’s cells cannot access this glucose for energy. This leads to a state of cellular starvation, where the body starts to break down fat and muscle for energy. It is not an efficient or safe long-term energy source for the body.
- Production of Ketones and Diabetic Ketoacidosis (DKA): The breakdown of fats leads to the production of acidic ketones. A high level of ketones in the body can lead to diabetic ketoacidosis, a serious and potentially life-threatening condition. Symptoms of DKA include nausea, vomiting, abdominal pain, rapid breathing, and in severe cases, unconsciousness.
- Long-Term Complications: Repeated episodes of high blood sugar without proper insulin management can lead to long-term complications associated with diabetes. That might include nerve damage, kidney damage, eye problems, heart disease, and stroke.
Therefore, individuals with Type 1 diabetes must take insulin as prescribed and monitor their blood sugar levels regularly to prevent these serious consequences.
What Are Some Diabetes Type 1 Treatments Without Insulin?
 It’s important to clarify that there are no treatments currently available that can replace insulin therapy in the management of Type 1 diabetes. Insulin is essential for life in individuals with Type 1 diabetes, as their bodies do not produce this vital hormone. However, several diabetes type 1 treatments without insulin can contribute to overall diabetes management:
It’s important to clarify that there are no treatments currently available that can replace insulin therapy in the management of Type 1 diabetes. Insulin is essential for life in individuals with Type 1 diabetes, as their bodies do not produce this vital hormone. However, several diabetes type 1 treatments without insulin can contribute to overall diabetes management:
Continuous Glucose Monitoring (CGM) Systems
Continuous Glucose Monitoring systems represent a significant advancement in diabetes management. They involve a small sensor inserted under the skin that measures glucose levels in the interstitial fluid. This data is then transmitted to a receiver or a smart device, providing real-time glucose readings. CGMs alert users to sudden changes in blood sugar levels. This is invaluable for preventing episodes of hyperglycemia (high blood sugar) and hypoglycemia (low blood sugar).
Insulin Pumps
Insulin pumps are devices that deliver insulin continuously through a catheter placed under the skin, mimicking the way a healthy pancreas would supply insulin. This method offers more precise control over blood sugar levels compared to traditional insulin injections. Pumps can be programmed to deliver varying amounts of insulin depending on factors like food intake and physical activity. They are particularly beneficial in achieving tighter blood sugar control and simplifying insulin management, especially in variable daily routines.
Dietary Management
Nutrition plays a crucial role in Type 1 diabetes management. A diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats, with careful monitoring of carbohydrate intake, can help stabilize blood sugar levels. Understanding how different foods affect blood sugar is key to adjusting insulin doses effectively. For instance, low-glycemic foods cause a slower, more gradual rise in blood glucose, making them a preferable choice for many people with diabetes.
Exercise
Regular physical activity is beneficial for those with Type 1 diabetes as it enhances insulin sensitivity, meaning the body uses insulin more efficiently. Exercise also helps in controlling blood glucose levels by using glucose for energy. However, it requires careful balance; physical activity can lower blood sugar levels. So monitoring glucose levels and adjusting insulin and carbohydrate intake accordingly is essential to prevent hypoglycemia.
Advanced Beta Cell Replacement Therapy
Beta-cell replacement therapies, like pancreas transplants or beta-cell encapsulation, aim to restore the body’s ability to produce insulin. In a pancreas transplant, a donor pancreas is transplanted to a person with diabetes. Beta-cell encapsulation involves enclosing insulin-producing cells in a protective barrier and implanting them in the body. These are promising areas but are complex and not widely available, often reserved for severe cases.
Immunotherapy
Immunotherapy in Type 1 diabetes focuses on modifying the immune system’s response to prevent or slow down the destruction of insulin-producing beta cells in the pancreas. This approach aims to preserve or restore the body’s insulin production. Several immunotherapy treatments are in clinical trials, exploring different methods to protect beta cells from the autoimmune attack characteristic of Type 1 diabetes.
Stem Cell Therapy
Stem cell therapy is a burgeoning field in the treatment of Type 1 diabetes. This approach involves using stem cells to create new insulin-producing cells, either through transplantation or by prompting the body to regenerate these cells itself. The goal is to replenish the body’s ability to produce its insulin. While research in this area has shown promise, it is still in the experimental stages and not yet a standard treatment option.
Each of these treatments and strategies offers potential benefits to individuals with Type 1 diabetes. But it’s crucial to remember that they are meant to complement, not replace, insulin therapy. Collaboration with healthcare professionals is essential in effectively integrating these approaches into a comprehensive diabetes management plan.
How Long Can Type 1 Go Without Insulin?
 The length of time a person with Type 1 diabetes can survive without insulin is highly variable and can be extremely dangerous. Type 1 diabetes is characterized by the pancreas’s inability to produce insulin, a hormone essential for regulating blood sugar levels. Without insulin, blood sugar levels can rapidly become uncontrolled.
The length of time a person with Type 1 diabetes can survive without insulin is highly variable and can be extremely dangerous. Type 1 diabetes is characterized by the pancreas’s inability to produce insulin, a hormone essential for regulating blood sugar levels. Without insulin, blood sugar levels can rapidly become uncontrolled.
- Initial Hours: In the initial hours without insulin, blood sugar levels will start to rise. This can lead to symptoms such as frequent urination, increased thirst, fatigue, and blurred vision.
- 24 Hours: Within about 24 hours without insulin, the body begins to break down fat as an alternative source of energy, leading to the production of ketones. The accumulation of ketones in the body can lead to a dangerous condition known as diabetic ketoacidosis (DKA).
- Diabetic Ketoacidosis (DKA): DKA can develop quickly, sometimes within 24 hours. Symptoms include nausea, vomiting, abdominal pain, rapid breathing, and confusion. DKA is a medical emergency that can lead to coma or even death if not treated promptly.
- Longer Durations: The longer a person with Type 1 diabetes goes without insulin, the greater the risk of severe and potentially fatal complications. The time frame can vary greatly among individuals, depending on factors like residual insulin production (if any), overall health, activity level, and the presence of other stressors or illnesses.
Individuals with Type 1 diabetes must understand that insulin is a life-saving medication, and its absence can lead to severe consequences in a relatively short period. They should never skip or delay insulin doses and always have a plan for obtaining insulin in emergencies.
Conclusion
In conclusion, while Type 1 diabetes management currently relies heavily on insulin therapy, there’s a wealth of additional strategies and emerging technologies that play a supportive role in improving overall health and quality of life for those with the condition. From continuous glucose monitoring systems that provide real-time insights into blood sugar levels to dietary and exercise plans tailored to individual needs, each element contributes to a personalized approach to diabetes type 1 treatments without insulin.
It’s important to remember that while these adjunct treatments and lifestyle changes are valuable, they complement rather than replace the need for insulin. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.