One of the most common and discomforting conditions with diabetes is diabetic neuropathy, particularly when it affects the feet. This condition, often manifesting as a burning sensation, can significantly impact one’s quality of life by limiting mobility and causing persistent discomfort. In this blog post, we’ll explore the various approaches to soothing and diabetic burning feet treatment caused by diabetic neuropathy, offering a ray of hope for those seeking relief.
Contents
Does Diabetes Cause Burning Feet?
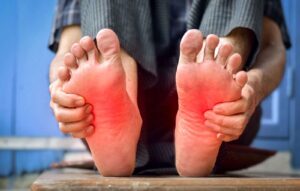 Yes, diabetes can cause a burning sensation in the feet, a condition often referred to as diabetic neuropathy. Diabetic neuropathy is a form of nerve damage that arises from high blood sugar levels associated with diabetes. Over time, elevated glucose levels can injure the nerves throughout the body, but the feet and legs are often the first areas to be affected.
Yes, diabetes can cause a burning sensation in the feet, a condition often referred to as diabetic neuropathy. Diabetic neuropathy is a form of nerve damage that arises from high blood sugar levels associated with diabetes. Over time, elevated glucose levels can injure the nerves throughout the body, but the feet and legs are often the first areas to be affected.
This nerve damage can lead to various symptoms, including pain, tingling, numbness, or a burning sensation in the feet. Eventually, making it a significant concern for many individuals living with diabetes. Proper management of blood sugar levels, alongside specific treatments for neuropathy, can help alleviate these symptoms.
Medical Approaches In Diabetic Burning Feet Treatment
In addressing the discomfort of burning feet caused by diabetic neuropathy, medical approaches play a crucial role. These treatments focus on controlling blood sugar levels to prevent further nerve damage and alleviate the pain and discomfort associated with this condition. Here’s an overview of the medical approaches used for diabetic burning feet treatment:
Blood Sugar Management
Effective control of blood glucose levels is foundational in preventing further nerve damage and mitigating symptoms of diabetic neuropathy.
- Monitoring: Frequent blood sugar testing and continuous glucose monitoring (CGM) devices help keep track of glucose levels in real time, allowing for immediate adjustments.
- Diet and Exercise: A balanced diet rich in nutrients, low in sugar, and unhealthy fats, combined with regular exercise, can significantly improve blood sugar control.
- Medication: Depending on the individual’s needs, oral medications or insulin therapy may be prescribed. These treatments require careful management to avoid hypoglycemia (low blood sugar levels) while preventing hyperglycemia (high blood sugar levels).
Prescription Medications for Neuropathy Pain
Pain management in diabetic neuropathy often involves medications that were initially developed for other conditions but are effective in treating nerve pain.
- Anticonvulsants: These medications stabilize electrical activity in the nerves and decrease neuropathic pain. Pregabalin and gabapentin are commonly prescribed and can be especially effective for nighttime pain.
- Antidepressants: Tricyclic antidepressants and serotonin-norepinephrine reuptake inhibitors (SNRIs) can interfere with pain signals in the brain, providing relief from neuropathic pain.
- Topical Treatments: Applied directly to the skin, these treatments can desensitize the area, providing temporary relief from pain. Capsaicin cream must be applied several times a day for the best effect. These lidocaine patches offer localized pain relief.
Over-the-counter (OTC) Remedies
For those with milder symptoms, OTC options may offer some relief.
- Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) can reduce inflammation and alleviate mild pain, though they’re often not strong enough for severe neuropathic pain.
- Supplements: Dietary supplements may support nerve health. Alpha-lipoic acid, for example, is an antioxidant that’s shown some efficacy in improving symptoms of neuropathy.
Physical Therapy
A tailored physical therapy program can support overall mobility and reduce pain.
- Exercise Plans: Custom exercises help strengthen the muscles, improve balance, and support the joints, potentially reducing the discomfort from neuropathy.
- Pain Management Techniques: Physical therapists may use TENS, massage, or thermal therapies as part of the treatment plan.
Electrical Nerve Stimulation
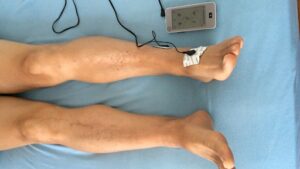 These techniques use electrical signals to disrupt or alter pain signaling pathways.
These techniques use electrical signals to disrupt or alter pain signaling pathways.
- TENS: A non-invasive method that can be used at home for pain management. The electrical impulses can block or reduce pain signals sent to the brain.
- Spinal Cord Stimulator: Used for severe, chronic pain cases where other treatments have failed, this device requires surgical implantation and emits electrical pulses directly to the spinal cord.
Alternative and Complementary Therapies
Interest in alternative therapies has grown, with some patients finding additional relief when these are added to conventional treatments.
- Acupuncture: This traditional Chinese medicine technique involves inserting thin needles into specific points on the body, potentially relieving pain by releasing endorphins and improving nerve function.
Managing diabetic neuropathy, particularly when it manifests as burning feet, requires a comprehensive approach. Collaboration between patients and healthcare providers is crucial to develop an effective treatment plan.
Home Remedies To Help In Diabetic Burning Feet
For individuals navigating the discomfort of diabetic burning feet, a blend of home remedies can serve as a comforting complement to medical treatments. These diabetic burning feet treatment options are rooted in the principles of easing pain, enhancing circulation, and promoting overall foot health. They are straightforward to implement and can offer tangible relief.
Cooling Strategies
The sensation of burning can often be mitigated through the application of cool temperatures. Regularly washing the feet with cool water can provide immediate, though temporary, relief. It’s a simple yet effective way to soothe the discomfort. Similarly, applying cool packs or a damp cloth chilled in the refrigerator (avoiding extreme cold to prevent shock to the skin) can help calm the fiery sensation. It’s essential to use these cooling methods judiciously to avoid reducing circulation further.
Foot Care Essentials
 Maintaining proper foot hygiene and care is paramount. Moisturizing the feet with hypoallergenic lotions can prevent the skin from becoming dry and cracked, which could worsen the discomfort. Furthermore, selecting footwear that provides support and comfort can prevent additional stress on sensitive feet. Shoes with a cushioned sole and sufficient room, paired with soft, seamless socks, can significantly enhance comfort.
Maintaining proper foot hygiene and care is paramount. Moisturizing the feet with hypoallergenic lotions can prevent the skin from becoming dry and cracked, which could worsen the discomfort. Furthermore, selecting footwear that provides support and comfort can prevent additional stress on sensitive feet. Shoes with a cushioned sole and sufficient room, paired with soft, seamless socks, can significantly enhance comfort.
Elevation for Relief
Elevating the feet above the heart level several times a day for about 15-20 minutes can aid in reducing swelling and improving circulation. This practice, combined with regular breaks to rest and elevate the feet, can contribute to alleviating the burning sensation.
The Role of Exercise
Engaging in regular, moderate exercise is beneficial for improving blood flow and managing blood glucose levels, both critical in reducing neuropathy symptoms. Activities like walking, swimming, or cycling are excellent options. These exercises enhance circulation without placing undue stress on the feet, offering a dual benefit of symptom relief and overall health improvement.
Dietary Adjustments
A balanced diet rich in nutrients supports optimal blood sugar control and can indirectly help manage neuropathy symptoms. Hydration plays a crucial role in maintaining circulation and overall health, while specific supplements, such as alpha-lipoic acid and B vitamins, might offer additional benefits in neuropathy management. Consulting with a healthcare provider before starting any new supplement is advisable to ensure it complements existing treatments.
Mind-Body Practices
Incorporating practices like yoga and tai chi can improve balance, reduce stress, and enhance well-being, potentially lessening the severity of neuropathy symptoms. Meditation and deep-breathing exercises offer a mental reprieve, helping to manage the psychological impact of living with chronic pain.
Warm Baths
A warm bath can soothe and relax the feet, improving circulation to the area. Care should be taken to ensure the water is not too hot, especially for those with reduced sensation in their feet, to prevent burns.
Essential Oils
For some, the application of diluted essential oils such as peppermint and lavender can provide relief. These oils have natural cooling and soothing properties and can be gently massaged into the feet. It’s important to test for allergies and consult a healthcare provider before incorporating essential oils into any treatment plan.
Avoiding Smoking
Smoking exacerbates circulation problems, which can intensify neuropathy pain. Quitting smoking is a significant step toward improving circulation and reducing symptoms, contributing to overall health improvement.
Integrating these home remedies into the daily routine can offer significant relief for those dealing with diabetic burning feet. However, these strategies should always be viewed as part of a broader treatment plan, developed in consultation with healthcare professionals, to ensure comprehensive care and management of diabetes and its associated symptoms.
Conclusion
Diabetic burning feet treatment involves a combination of medical treatments, lifestyle changes, and home remedies. From maintaining proper blood sugar levels and using prescribed medications to adopting cooling strategies, regular exercise, and mindful dietary choices, there are many ways to alleviate the discomfort. Incorporating gentle exercises, elevating the feet, and even using cool or warm baths can provide relief.
While these methods can help soothe burning sensations and improve overall foot health, it’s essential to work closely with healthcare professionals. Remember, every small step towards managing your symptoms can lead to a significant improvement in your quality of life. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.

