Whether you are dealing with diabetes or experiencing elevated blood sugar for other reasons, it’s essential to equip yourself with knowledge and strategies to navigate this health concern effectively. In this blog, we’ll explore the intricacies of high glucose and practical approaches for high glucose treatment. Join us on a journey towards better health and well-being as we delve into the world of managing and thriving despite high glucose levels.
Contents
How Do I Identify High Glucose Levels?
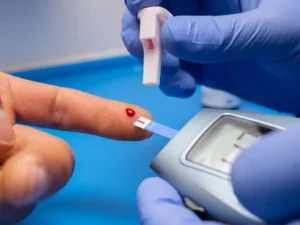 Identifying high glucose levels typically involves recognizing the signs and symptoms associated with hyperglycemia. If you suspect you may have high glucose or are at risk for diabetes, it’s essential to consult with a healthcare professional for proper evaluation and diagnosis. Here are common signs and methods for identifying high glucose:
Identifying high glucose levels typically involves recognizing the signs and symptoms associated with hyperglycemia. If you suspect you may have high glucose or are at risk for diabetes, it’s essential to consult with a healthcare professional for proper evaluation and diagnosis. Here are common signs and methods for identifying high glucose:
- Frequent Urination (Polyuria): Excessive glucose in the blood can lead to increased urine production, causing more frequent trips to the bathroom.
- Excessive Thirst (Polydipsia): Increased urination can result in dehydration, leading to heightened feelings of thirst.
- Extreme Hunger (Polyphagia): Despite eating, individuals with high glucose levels may experience persistent feelings of hunger and not feel satisfied after meals.
- Unexplained Weight Loss: When the body cannot use glucose properly, it may start breaking down muscle and fat for energy, resulting in weight loss.
- Fatigue and Weakness: Insufficient glucose utilization can lead to feelings of fatigue and weakness.
- Blurred Vision: High glucose levels can affect the fluid levels in the lenses of the eyes, causing blurred vision.
- Slow Healing of Wounds: Elevated blood sugar can impair the body’s ability to heal, leading to delayed wound healing and an increased risk of infections.
- Recurrent Infections: High glucose levels may weaken the immune system, making individuals more susceptible to infections, particularly in the skin, urinary tract, and other areas.
- Tingling or Numbness in Extremities: Prolonged high glucose levels can damage nerves. This leads to sensations of tingling or numbness, particularly in the hands and feet.
- Mood Changes: Fluctuations in blood sugar levels can impact mood, leading to irritability and difficulty concentrating.
If you experience these symptoms, especially if they persist or worsen over time, it is crucial to seek medical attention promptly. A healthcare professional can perform blood tests, such as fasting blood glucose or hemoglobin A1c, to assess your glucose levels and determine if further evaluation or intervention is needed.
What Are Some Medical Approaches To High Glucose Treatment?
 Medical approaches to high glucose treatment often depend on the underlying cause, with a primary focus on managing conditions such as diabetes. The goal is to achieve and maintain blood glucose levels within a target range to prevent complications. Here are some common medical approaches to high glucose treatment:
Medical approaches to high glucose treatment often depend on the underlying cause, with a primary focus on managing conditions such as diabetes. The goal is to achieve and maintain blood glucose levels within a target range to prevent complications. Here are some common medical approaches to high glucose treatment:
Oral Medications
Oral medications are commonly prescribed for individuals with type 2 diabetes, a condition characterized by insulin resistance or insufficient insulin production. Metformin, a widely used medication, improves insulin sensitivity in tissues and reduces glucose production by the liver. Sulfonylureas stimulate the pancreas to release more insulin, while DPP-4 inhibitors increase the lifespan of incretin hormones. This regulates insulin and glucagon secretion.
Insulin Therapy
Insulin therapy is a cornerstone of treatment for individuals with type 1 diabetes. In this, the body doesn’t produce insulin, and some with type 2 diabetes, may require additional insulin support. Insulin can be administered through injections or an insulin pump. Different types of insulin are available to mimic the body’s natural insulin production patterns. Ultimately, providing both basal (background) and bolus (mealtime) coverage. The goal of insulin therapy is to maintain blood glucose within a target range, preventing hyperglycemia and minimizing the risk of complications.
GLP-1 Receptor Agonists
GLP-1 receptor agonists are injectable medications that mimic the action of the natural incretin hormone GLP-1. By stimulating insulin release and inhibiting glucagon production, these medications help lower blood glucose levels. GLP-1 receptor agonists also slow down gastric emptying, promoting a feeling of fullness and contributing to weight loss. They are commonly prescribed for individuals with type 2 diabetes who may benefit from the multifaceted actions of this class of medications.
SGLT-2 Inhibitors
Sodium-glucose cotransporter-2 (SGLT-2) inhibitors are oral medications that act on the kidneys to reduce glucose reabsorption. This further leads to increased glucose excretion in the urine. By promoting the elimination of excess glucose, these medications help lower blood sugar levels. SGLT-2 inhibitors are often used in the treatment of type 2 diabetes and may also have additional cardiovascular and renal benefits. However, they are not suitable for individuals with certain kidney conditions.
DPP-4 Inhibitors
DPP-4 inhibitors are another class of oral medications used in the treatment of type 2 diabetes. They work by blocking the action of an enzyme called dipeptidyl peptidase-4 (DPP-4), which rapidly degrades incretin hormones. By inhibiting DPP-4, these medications prolong the activity of incretins, such as GLP-1. This stimulates insulin release and reduces glucagon production. DPP-4 inhibitors are taken orally and are typically well-tolerated with fewer side effects compared to some other diabetes medications.
Combination Therapies
In many cases, a single medication may not be sufficient to manage high glucose levels effectively. Combination therapies involve the use of two or more medications with different mechanisms of action to address multiple aspects of glucose regulation. For instance, a healthcare provider might prescribe a combination of metformin with a sulfonylurea or a DPP-4 inhibitor to achieve better glycemic control.
Continuous Glucose Monitoring (CGM)
Continuous Glucose Monitoring (CGM) systems provide real-time information about glucose levels throughout the day and night. A small sensor inserted under the skin measures glucose levels in the interstitial fluid. The data is transmitted to a device that displays the readings. CGM allows individuals and healthcare providers to track patterns, identify trends, and make timely adjustments to medication regimens, diet, and lifestyle. This technology is particularly beneficial for those who require precise and dynamic control over their blood glucose levels.
Artificial Pancreas Systems
Artificial pancreas systems, also known as closed-loop systems, represent a cutting-edge technology in diabetes management. These systems integrate CGM with an insulin pump, creating an automated approach to insulin delivery. The device continually monitors glucose levels and adjusts insulin delivery in real-time, mimicking the function of a healthy pancreas. Artificial pancreas systems aim to provide better blood glucose control and reduce the burden of constant decision-making for individuals with diabetes.
It’s important to note that treatment plans are individualized based on factors such as the type of diabetes, overall health, lifestyle, and personal preferences. Regular monitoring of blood glucose levels, medication adherence, and close collaboration with healthcare professionals are critical for successful high glucose management.

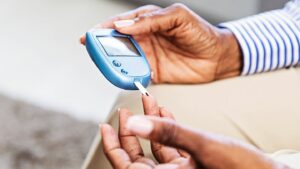
 If you have diabetes or are experiencing persistent high glucose levels, it’s crucial to consult with your healthcare provider. They can provide personalized advice, adjust medications if necessary, and guide you on the most appropriate strategies for your specific situation.
If you have diabetes or are experiencing persistent high glucose levels, it’s crucial to consult with your healthcare provider. They can provide personalized advice, adjust medications if necessary, and guide you on the most appropriate strategies for your specific situation.