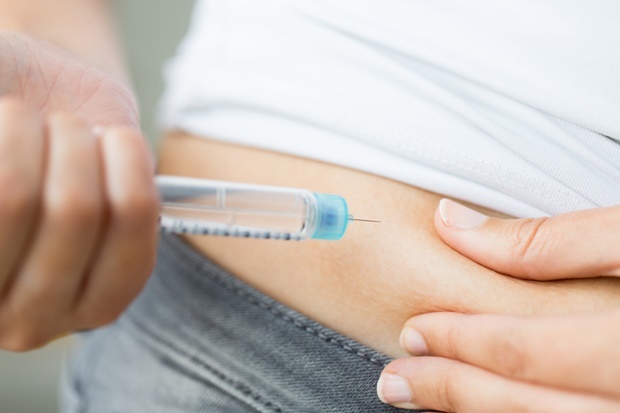
Living with diabetes requires a multifaceted approach to managing blood sugar levels, and for many individuals, injectable medications play a crucial role in their treatment plan. As the landscape of diabetes management continues to evolve, so do the options available for injectable medications. In this comprehensive guide, we will explore the various injectable diabetes medications, shedding light on their mechanisms, benefits, and considerations.
Contents
What Are The Best Injectable Diabetes Medications?
 The choice of the best injectable diabetes medication depends on various factors, including the individual’s specific needs, lifestyle, and overall health. Different medications work in different ways to help manage blood sugar levels. Here are some of the commonly prescribed and well-regarded injectable diabetes medications:
The choice of the best injectable diabetes medication depends on various factors, including the individual’s specific needs, lifestyle, and overall health. Different medications work in different ways to help manage blood sugar levels. Here are some of the commonly prescribed and well-regarded injectable diabetes medications:
Insulin
Insulin is a fundamental and essential injectable medication for individuals with diabetes. Rapid-acting insulins, such as insulin lispro and insulin aspart, are designed to address postprandial blood sugar spikes. And, making them suitable for use just before or with meals. Short-acting insulin (Regular insulin) takes effect within 30 minutes and lasts for several hours, providing coverage for a longer duration. Intermediate-acting insulin (NPH insulin) has a more extended duration of action. Eventually makes it useful for maintaining blood sugar control between meals.
GLP-1 Receptor Agonists
GLP-1 receptor agonists, such as liraglutide (Victoza), dulaglutide (Trulicity), and semaglutide (Ozempic), are injectable medications that mimic the effects of GLP-1, a hormone that enhances insulin secretion, reduces glucagon production, and slows stomach emptying. These medications are typically administered once a week, offering convenience and potentially contributing to weight loss in addition to blood sugar control. GLP-1 receptor agonists are often considered for people with type 2 diabetes who may benefit from both glycemic control and weight management.
GLP-1 Receptor Agonist/Insulin Combinations
Combining the benefits of long-acting insulin with the effects of a GLP-1 receptor agonist, medications like insulin glargine/lixisenatide (Soliqua) and insulin degludec/liraglutide (Xultophy) provide a comprehensive approach to diabetes management. These combination products offer both basal insulin coverage for overall glucose control and the additional advantage of controlling postprandial glucose levels. By addressing multiple aspects of glucose regulation, these combination therapies can simplify treatment regimens for individuals with diabetes.
Amylinomimetic
Pramlintide (Symlin) is an injectable medication classified as an amylinomimetic, as it mimics the actions of amylin, a hormone that works in conjunction with insulin to regulate blood sugar levels. Typically used in combination with insulin therapy, pramlintide slows gastric emptying, reduces postprandial glucose levels, and helps minimize the risk of hypoglycemia. By providing an additional layer of control, pramlintide can be particularly beneficial for individuals who struggle to achieve desired blood sugar targets with insulin alone.
SGLT-2 Inhibitors
While not administered through injection, SGLT-2 inhibitors, including empagliflozin (Jardiance), canagliflozin (Invokana), and dapagliflozin (Farxiga), play a significant role in diabetes management. These oral medications work by inhibiting glucose reabsorption in the kidneys, promoting the excretion of excess glucose in the urine. SGLT-2 inhibitors are often prescribed in conjunction with injectable medications. And can contribute to both glycemic control and cardiovascular benefits. Their inclusion in a comprehensive diabetes treatment plan underscores the importance of a multifaceted approach to managing this complex condition.
It’s important to note that the “best” medication varies for each individual. Factors such as the type of diabetes, comorbidities, potential side effects, and personal preferences all play a role in the decision-making process. Healthcare professionals work closely with individuals with diabetes to tailor a treatment plan. This further meets their specific needs and helps achieve optimal blood sugar control.
Which Injectable Diabetes Medication Should I Opt For?
 The choice of injectable diabetes medication depends on various factors, and it is a decision that should be made in consultation with your healthcare provider. Here are some considerations to help guide your discussion with your healthcare team:
The choice of injectable diabetes medication depends on various factors, and it is a decision that should be made in consultation with your healthcare provider. Here are some considerations to help guide your discussion with your healthcare team:
Type of Diabetes
- Type 1 Diabetes: People with type 1 diabetes typically require insulin as their primary injectable medication. Different types of insulin and delivery methods may be considered based on individual needs and lifestyle.
- Type 2 Diabetes: Individuals with type 2 diabetes may have a broader range of options, including GLP-1 receptor agonists, insulin, or combination therapies. The specific medication prescribed will depend on factors such as blood sugar levels, other health conditions, and personal preferences.
Blood Sugar Control Goals
If your primary concern is achieving better postprandial blood sugar control, medications like rapid-acting insulin or GLP-1 receptor agonists may be considered. For comprehensive blood sugar management throughout the day, a combination therapy involving basal insulin and GLP-1 receptor agonists might be an option.
Weight Management Goals
If weight loss is a priority, GLP-1 receptor agonists are known to be associated with weight reduction in addition to blood sugar control. Certain combination therapies, such as those pairing GLP-1 receptor agonists with insulin, may provide glycemic control while potentially mitigating weight gain.
Frequency of Injections
Consider your comfort level with injections and the frequency with which you are willing to administer medication. Some medications, like certain GLP-1 receptor agonists, are administered once a week, while others, such as insulin, may require more frequent injections.
Lifestyle Considerations
Think about your daily routine, work schedule, and lifestyle. Some medications may offer more flexibility in terms of timing and administration, while others may require more structured meal and injection schedules.
Cost and Insurance Coverage
Check with your insurance provider to understand the coverage for different medications. Cost can be a significant factor in decision-making, and there may be generic or more cost-effective options available.
Always consult with your healthcare provider to determine the most suitable injectable diabetes medication for your individual needs. Your healthcare team will consider various factors to tailor a treatment plan that aligns with your goals, lifestyle, and overall health.
What Are The Pros And Cons Of Injectable Diabetes Medications?
 Injectable diabetes medications, including insulin and other injectables like GLP-1 receptor agonists, offer several benefits and considerations. It’s important to discuss these pros and cons with your healthcare provider to determine the most appropriate treatment plan for your individual needs. Here’s an overview:
Injectable diabetes medications, including insulin and other injectables like GLP-1 receptor agonists, offer several benefits and considerations. It’s important to discuss these pros and cons with your healthcare provider to determine the most appropriate treatment plan for your individual needs. Here’s an overview:
Pros
- Effective Blood Sugar Control: Injectable medications, especially insulin, are highly effective in controlling blood sugar levels. They provide a direct way to regulate glucose in the bloodstream.
- Customization and Flexibility: Injectable medications can be customized to meet individual needs. Healthcare providers can adjust dosages and combinations to achieve optimal blood sugar control.
- Comprehensive Approach: Some injectable medications, such as GLP-1 receptor agonists, offer a multifaceted approach by not only controlling blood sugar but also contributing to weight loss and reducing cardiovascular risk factors.
- Long-Acting Options: Long-acting insulins and certain GLP-1 receptor agonists require less frequent injections. And, providing convenience for individuals who prefer a less intensive injection schedule.
- Treatment of Various Diabetes Types: Injectable medications are used in the management of both type 1 and type 2 diabetes. Also, offering versatile options for a broad range of individuals.
Cons
- Injection Site Reactions: Some individuals may experience pain, redness, or irritation at the injection site. Rotating injection sites and proper technique can help minimize these reactions.
- Risk of Hypoglycemia: Injectable medications, particularly insulin, can pose a risk of hypoglycemia (low blood sugar). Careful monitoring and adjustment of dosages are necessary to avoid this potential complication.
- Weight Gain: Certain insulin formulations may be associated with weight gain. This can be a concern, especially for individuals with type 2 diabetes who are aiming for weight management.
- Treatment Intensification: As diabetes progresses, treatment plans may need to be intensified, potentially leading to the addition of more medications or higher doses. This can complicate the management approach.
- Fear or Anxiety of Injections: Some individuals may have a fear of needles or anxiety associated with injections. This psychological aspect can impact adherence to the treatment plan.
- Digestive Side Effects: GLP-1 receptor agonists, while generally well-tolerated, may cause digestive side effects. Such as nausea and diarrhea in some individuals. These side effects often improve over time.
It’s crucial to weigh the pros and cons in the context of your specific health status, lifestyle, and preferences. Regular communication with your healthcare provider is essential to address any concerns, monitor for side effects, and make necessary adjustments to your diabetes management plan.
Conclusion
In conclusion, navigating the world of injectable diabetes medications offers a range of options for managing blood sugar levels effectively. From insulin therapies providing precise control to GLP-1 receptor agonists offering multifaceted benefits, each medication has its pros and cons. The key lies in personalized decision-making guided by factors such as lifestyle, preferences, and health goals. Making sure you have regular communication with healthcare providers is crucial to finding the most suitable injectable medication.
Ultimately, it ensures effective diabetes management while considering individual needs and promoting overall well-being. Remember, you’re not alone on this journey—your healthcare team is there to support you in making informed choices and achieving the best possible outcomes in your diabetes care. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.