Insulin, a hormone produced by the pancreas, is crucial in regulating blood sugar (glucose) levels. In the absence of natural insulin production, people with type 1 diabetes need to administer insulin externally to control their blood sugar. In this blog, we’ll delve into the various aspects of insulin therapy for type 1 diabetes, including the types of insulin, administration methods, and advancements in insulin delivery technology.
Contents
What is Insulin Therapy?
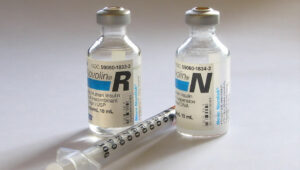
Insulin therapy is a medical treatment for individuals with diabetes, particularly those with type 1 diabetes and some cases of type 2 diabetes. It involves the administration of insulin, a hormone essential for regulating blood sugar (glucose) levels in the body. Insulin allows cells to absorb glucose from the bloodstream, providing the necessary energy to function properly.
In people with type 1 diabetes, the immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. As a result, the body cannot produce its insulin, necessitating external insulin replacement. In some cases of type 2 diabetes, the body may not effectively use the insulin it produces and insulin therapy may also be prescribed.
Types of Insulin Therapy for Type 1 Diabetes
Insulin therapy is a cornerstone in the management of type 1 diabetes, a chronic condition where the immune system attacks and destroys the insulin-producing beta cells in the pancreas. The goal of insulin therapy in type 1 diabetes is to mimic the body’s natural insulin secretion to regulate blood glucose levels. There are several types of insulin with varying onset, peak, and duration characteristics, allowing for a personalized approach to meet individual needs. Here are the main types of insulin used in type 1 diabetes therapy:
Rapid-Acting Insulin:
- Examples: Insulin lispro, insulin aspart, and insulin glulisine.
- Onset: Rapid-acting insulin starts working within 15 minutes of administration.
- Peak: The peak effectiveness occurs around 1-2 hours after administration.
- Duration: The effects last for about 2-4 hours.
- Usage: Typically taken just before or right after meals to manage post-meal glucose spikes.
Short-Acting Insulin:
- Example: Regular insulin (R insulin).
- Onset: Short-acting insulin starts working within 30 minutes.
- Peak: Peak effectiveness is observed between 2-3 hours post-administration.
- Duration: The effects can last up to 6 hours.
- Usage: Usually taken about 30 minutes before meals to cover the rise in blood glucose associated with eating.
Intermediate-Acting Insulin:
- Example: NPH (Neutral Protamine Hagedorn) insulin.
- Onset: Intermediate-acting insulin has a slower onset, typically within 2-4 hours.
- Peak: Peak effectiveness occurs between 4-12 hours.
- Duration: The effects can last up to 18 hours.
- Usage: Often used to provide background or basal insulin levels between meals and overnight.
Long-Acting Insulin:
- Examples: Insulin glargine, insulin detemir, and insulin degludec.
- Onset: Long-acting insulin has a gradual onset, starting within 1-2 hours.
- Peak: It has a minimal peak, providing a steady release over an extended period.
- Duration: The effects can last anywhere from 18 to 24 hours.
- Usage: Used to maintain a constant level of insulin in the body, typically taken once or twice a day.
It’s common for individuals with type 1 diabetes to use a combination of these insulin types, known as basal-bolus insulin therapy. This approach involves using long-acting insulin for baseline insulin needs (basal) and rapid or short-acting insulin to cover mealtime spikes in blood glucose (bolus).
Methods of Insulin Administration
Insulin can be administered through various methods, and the choice of method depends on individual preferences, lifestyle, and healthcare provider recommendations. The primary methods of insulin administration include:
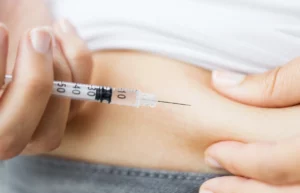
Subcutaneous Injections:
- Description: Subcutaneous injections involve injecting insulin into the fatty tissue just beneath the skin.
- Devices: Subcutaneous injections can be administered using insulin syringes, insulin pens, or insulin pumps.
- Common Practice: This is the most common and traditional method of insulin delivery.
- Rotation of Injection Sites: Regular rotation of injection sites is recommended to prevent the development of lumps, skin changes, or lipohypertrophy (thickened fatty tissue).
Insulin Pens:
- Description: Insulin pens are pen-shaped devices that contain pre-filled insulin cartridges or replaceable insulin cartridges.
- Advantages: They offer a convenient and discreet way to administer insulin, with built-in dose settings for precise delivery.
- Disposable and Reusable: Insulin pens come in disposable and reusable forms.
- Ease of Use: Particularly beneficial for individuals who may have difficulty using a syringe.
Insulin Pumps:
- Description: Insulin pumps are small, programmable devices that continuously deliver a basal (background) dose of insulin throughout the day and can provide additional bolus doses at mealtime.
- Continuous Delivery: Mimics the function of a healthy pancreas more closely by delivering a steady supply of insulin.
- Adjustable Doses: Allows for precise adjustments of insulin doses based on individual needs.
- Subcutaneous Infusion: Insulin is delivered through a small tube (cannula) placed under the skin.
- Wireless Connectivity: Some modern pumps have Bluetooth capabilities, enabling data sharing with smartphones or other devices.
Inhaled Insulin:
- Description: Inhaled insulin involves inhaling a fine powder containing insulin particles into the lungs.
- Device: Administered using a specialized inhaler device.
- Advantages: Offers an alternative to injections, particularly for individuals who may have needle phobia.
- Limitations: Not suitable for everyone, and it may have restrictions based on certain health conditions.
Jet Injectors:
- Description: Jet injectors use high-pressure air to deliver insulin through the skin without using a needle.
- Less Common: While they were used in the past, jet injectors are less common today due to the availability of other more user-friendly options.
How Many Units of Insulin Is Normal?
Normal insulin levels can vary depending on various factors such as age, weight, diet, and individual health conditions. However, here are some general guidelines:
Fasting Insulin Levels:
- Normal fasting insulin levels typically range from 5 to 15 microinternational units per milliliter (uIU/mL) or 35 to 105 picomoles per liter (pmol/L).
- These levels may vary slightly depending on the laboratory and the units used for measurement.
Postprandial Insulin Levels (after meals):
- After a meal, insulin levels typically rise to facilitate the uptake of glucose into cells for energy production.
- Postprandial insulin levels can vary widely depending on the composition and size of the meal, but they generally should not exceed 30 uIU/mL.
Insulin Sensitivity:
- Insulin sensitivity refers to how efficiently the body’s cells respond to insulin. Higher sensitivity generally means lower insulin levels are needed to maintain normal blood sugar levels.
- Individuals with insulin resistance may have higher fasting and postprandial insulin levels to compensate for decreased insulin sensitivity.
Insulin Dosage for Diabetes Management:
For individuals with diabetes who require insulin therapy, the dosage can vary widely based on factors such as:
- Type of diabetes (Type 1, Type 2, gestational diabetes).
- Body weight.
- Blood sugar levels (target range).
- Insulin sensitivity.
- Other medical conditions.
Dosages are typically measured in units (such as units of rapid-acting insulin before meals or long-acting insulin for basal coverage throughout the day).
Consulting Healthcare Professionals:
- It’s essential for individuals with diabetes or those concerned about their insulin levels to consult healthcare professionals, such as endocrinologists, diabetologists, or primary care physicians.
- These professionals can conduct tests to measure insulin levels accurately, interpret the results in the context of the individual’s health status, and provide personalized recommendations for management and treatment.
In conclusion, while there are general ranges for normal insulin levels, individual variation is significant. For individuals with diabetes, proper management involves maintaining blood sugar levels within target ranges through medication, diet, exercise, and regular monitoring under the guidance of healthcare professionals.
Key Considerations in Insulin Therapy in Type 1 Diabetes
Insulin therapy is a crucial aspect of managing type 1 diabetes, and several key considerations play a vital role in optimizing its effectiveness. Here are important factors to consider when undertaking insulin therapy for type 1 diabetes:
Individualized Treatment Plans:
- Personalized Approach: Type 1 diabetes varies among individuals, and there is no one-size-fits-all solution. Tailor insulin therapy plans based on factors such as age, lifestyle, activity level, and overall health.
Basal-Bolus Regimen:
- Balancing Act: Utilize a basal-bolus insulin regimen, incorporating both long-acting (basal) and rapid-acting (bolus) insulin to mimic the body’s natural insulin secretion pattern.
- Mealtime Coverage: Adjust bolus insulin doses to cover meals and snacks, considering carbohydrate intake and blood glucose levels.
Blood Glucose Monitoring:
- Frequent Monitoring: Regularly monitor blood glucose levels to understand patterns and make informed insulin dosage adjustments.
- Continuous Glucose Monitoring (CGM): Consider using CGM systems for real-time glucose data, providing more comprehensive insights into glucose fluctuations.
Insulin Types and Formulations:
- Understanding Insulin Types: Familiarize yourself with the characteristics of rapid-acting, short-acting, intermediate-acting, and long-acting insulins.
- Flexible Adjustments: Adjust the types and timings of insulin based on daily routines, activity levels, and specific needs.
Injection Techniques:
- Proper Administration: Ensure correct injection techniques, including the rotation of injection sites to prevent lipohypertrophy and skin changes.
- Injection Timing: Consistently administer insulin at the recommended times to maintain consistent blood glucose control.
Insulin Pump Considerations:
- Continuous Delivery: Understand the benefits of insulin pumps, which provide a continuous supply of basal insulin and bolus doses at mealtime.
- Adjustable Basal Rates: Take advantage of programmable basal rates on insulin pumps for more precise insulin delivery.
Hypoglycemia Prevention:
- Recognition and Response: Be aware of the symptoms of hypoglycemia (low blood sugar) and have a plan for prompt and appropriate responses.
- Adjusting Insulin Doses: Adjust insulin doses cautiously to prevent hypoglycemia, especially during periods of increased physical activity.
Lifestyle Considerations:
- Dietary Choices: Align insulin dosages with dietary choices, considering the impact of carbohydrates on blood glucose levels.
- Physical Activity: Adjust insulin doses based on physical activity levels to prevent hypoglycemia and maintain glucose stability.
Conclusion
Insulin therapy is the cornerstone of managing type 1 diabetes, providing individuals with the means to lead active and healthy lives. With the availability of various insulin types, delivery methods, and technological advancements, the landscape of diabetes management continues to evolve. As research progresses, we can anticipate even more innovative solutions to enhance insulin therapy’s precision, convenience, and effectiveness for individuals with type 1 diabetes.
Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.

