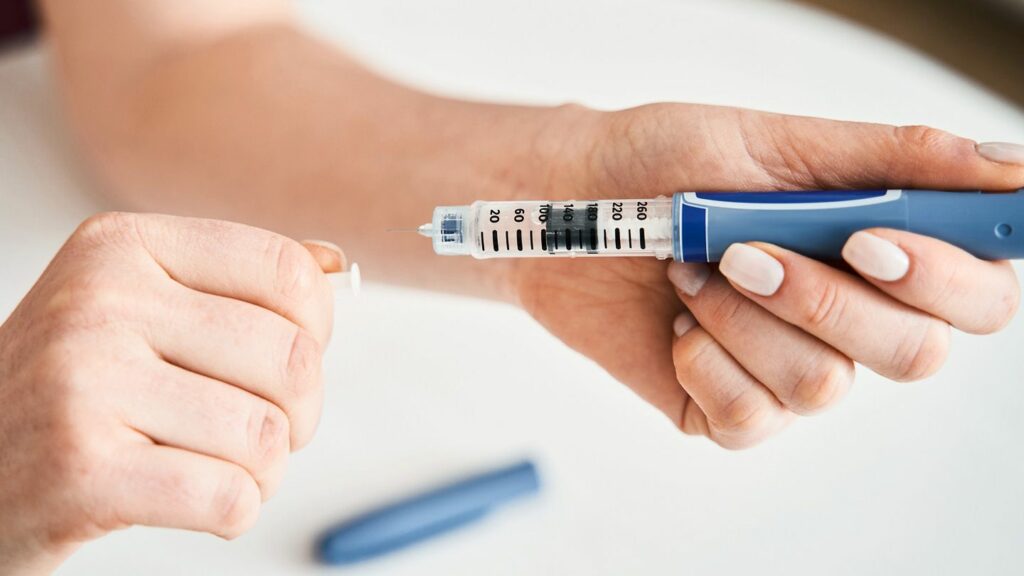
Juvenile diabetes, also known as type 1 diabetes, can present unique challenges for both children and their families. Managing blood sugar levels, navigating insulin regimens, and addressing the emotional aspects of this chronic condition requires a multifaceted approach. In this blog, we aim to provide valuable insights, practical tips, and the latest advancements in juvenile diabetes treatment to empower individuals and their loved ones on their journey toward a healthier and more fulfilling life.
Contents
Is Juvenile Diabetes Common?
 Juvenile diabetes, also known as type 1 diabetes (T1D), is less common than its counterpart, type 2 diabetes. However, it is still a prevalent chronic condition, particularly among children and adolescents. While the overall prevalence varies across populations, studies indicate that approximately 1 in 500 children and adolescents worldwide are diagnosed with type 1 diabetes. The onset of type 1 diabetes typically occurs before the age of 20, with a peak incidence around puberty.
Juvenile diabetes, also known as type 1 diabetes (T1D), is less common than its counterpart, type 2 diabetes. However, it is still a prevalent chronic condition, particularly among children and adolescents. While the overall prevalence varies across populations, studies indicate that approximately 1 in 500 children and adolescents worldwide are diagnosed with type 1 diabetes. The onset of type 1 diabetes typically occurs before the age of 20, with a peak incidence around puberty.
Despite its lower prevalence compared to type 2 diabetes, the impact of juvenile diabetes can be significant. Because it requires lifelong management and requires careful attention to blood sugar levels, insulin administration, and lifestyle factors. Juvenile diabetes is characterized by the immune system’s destruction of insulin-producing beta cells in the pancreas, leading to a deficiency of insulin, a hormone crucial for regulating blood sugar.
While the exact causes remain unclear, genetic factors and environmental triggers are believed to contribute to the development of type 1 diabetes. Although the prevalence of juvenile diabetes is lower than type 2 diabetes, its impact on the lives of affected individuals and their families is substantial.
What Are Some Best Juvenile Diabetes Treatment Options?
Juvenile diabetes, or type 1 diabetes (T1D), is a chronic condition that requires lifelong management. The primary focus of treatment for juvenile diabetes is to maintain blood sugar levels within a target range, as the body’s inability to produce insulin requires external insulin administration. Here are some key components of juvenile diabetes treatment:
Insulin Therapy
Insulin therapy is the cornerstone of juvenile diabetes treatment due to the body’s inability to produce insulin. Multiple Daily Injections (MDI) involve administering fast-acting insulin before meals and long-acting insulin for baseline coverage. Insulin pumps, another common approach, continuously deliver insulin with additional doses for meals. Pumps offer flexibility, allowing users to adjust insulin delivery based on factors like physical activity and meals, closely mimicking the body’s natural insulin release.
Blood Sugar Monitoring
Regular blood sugar monitoring is essential for effective diabetes management. Frequent testing helps individuals understand their glucose levels and make informed decisions about insulin doses, diet, and lifestyle. Continuous Glucose Monitoring (CGM) systems provide real-time data on glucose trends, enabling a more comprehensive view of blood sugar dynamics. CGMs offer alerts for potential highs or lows, aiding proactive adjustments to maintain stable blood sugar levels.
Meal Planning and Nutrition
Successful juvenile diabetes management involves careful meal planning. Carbohydrate counting is a common practice, allowing individuals to adjust insulin doses based on the amount of carbohydrates consumed. A balanced diet that includes a mix of carbohydrates, proteins, and fats helps stabilize blood sugar levels. Nutrition education is a crucial component, empowering individuals to make informed choices about their diet and overall well-being.
Regular Exercise
 Physical activity is beneficial for individuals with juvenile diabetes, contributing to overall health and aiding in blood sugar regulation. Exercise increases insulin sensitivity, allowing the body to use insulin more effectively. However, it’s essential to balance physical activity with insulin and nutrition to prevent glucose fluctuations. Tailoring exercise plans to individual needs, considering factors like the type and duration of activity, is crucial for maintaining optimal blood sugar control.
Physical activity is beneficial for individuals with juvenile diabetes, contributing to overall health and aiding in blood sugar regulation. Exercise increases insulin sensitivity, allowing the body to use insulin more effectively. However, it’s essential to balance physical activity with insulin and nutrition to prevent glucose fluctuations. Tailoring exercise plans to individual needs, considering factors like the type and duration of activity, is crucial for maintaining optimal blood sugar control.
Education and Support
Comprehensive education on diabetes management is paramount. Understanding the condition, treatment options, and lifestyle adjustments empowers individuals and their families to navigate the challenges of juvenile diabetes confidently. Support groups, counseling, and educational resources provide emotional and practical assistance, fostering a sense of community and resilience.
Emerging Technologies
Ongoing technological advancements aim to enhance diabetes care. Artificial pancreas systems and closed-loop insulin delivery represent cutting-edge technologies that automate insulin adjustments based on real-time glucose data. These innovations offer the potential to simplify diabetes management, reduce the burden on individuals, and improve overall treatment outcomes.
Research and Clinical Trials
Active participation in ongoing research and clinical trials is a promising avenue for those with juvenile diabetes. These endeavors explore new treatment modalities, potential cures, and improved management strategies. By staying informed about and contributing to advancements in diabetes care, individuals can play a role in shaping the future of juvenile diabetes treatment and potentially gain access to novel therapeutic approaches.
It’s important with juvenile diabetes to work closely with healthcare professionals to tailor their treatment plan to their specific needs, considering factors like age, lifestyle, and individual response to insulin. Regular monitoring, a healthy lifestyle, and staying informed about advancements in diabetes care are essential components of effective juvenile diabetes management.
What Are The Lifestyle Changes That Can Help?
 Lifestyle changes play a crucial role in juvenile diabetes treatment (type 1 diabetes) effectively. Here are key lifestyle modifications that can contribute to better blood sugar control and overall well-being:
Lifestyle changes play a crucial role in juvenile diabetes treatment (type 1 diabetes) effectively. Here are key lifestyle modifications that can contribute to better blood sugar control and overall well-being:
Healthy Eating Habits
Adopting a balanced and nutritious diet is fundamental. Focus on a variety of foods, including fruits, vegetables, lean proteins, and whole grains. Carbohydrate counting helps individuals manage insulin doses more accurately, and spreading meals throughout the day can prevent blood sugar spikes.
Consistent Meal Timing
Establishing regular meal times and spacing meals evenly throughout the day contributes to stable blood sugar levels. Consistency in meal timing helps synchronize insulin administration with food intake, reducing the risk of fluctuations.
Hydration
Staying adequately hydrated is essential for overall health and can assist in maintaining stable blood sugar levels. Water is the best choice for hydration, and individuals should monitor their fluid intake. Especially if they are incorporating sugary beverages or sports drinks.
Stress Management
Chronic stress can impact blood sugar levels. Developing effective stress management techniques, such as mindfulness, meditation, deep breathing, or engaging in hobbies, can positively influence both physical and emotional well-being.
Adequate Sleep
Prioritizing sufficient and quality sleep is crucial. Lack of sleep can affect blood sugar control and insulin sensitivity. Aim for a consistent sleep schedule and create a relaxing bedtime routine to promote restful sleep.
Regular Monitoring and Record-Keeping
Keeping a log of blood sugar levels, meals, physical activity, and insulin doses helps individuals and healthcare providers identify patterns and make informed adjustments to the treatment plan. This proactive approach can lead to better control over blood sugar levels.
Regular Medical Check-ups
Scheduled visits to healthcare professionals are essential for monitoring overall health and diabetes management. Regular check-ups allow for the assessment of blood sugar control, adjustments to treatment plans, and addressing any emerging concerns promptly.
Alcohol Moderation
If consuming alcohol, it’s important to do so in moderation and be mindful of its impact on blood sugar levels. Alcohol can lead to fluctuations, and individuals should monitor their responses and coordinate alcohol consumption with their healthcare team.
These lifestyle changes, when implemented as part of a comprehensive diabetes management plan, can significantly contribute to better health outcomes for individuals with juvenile diabetes. Individuals must work closely with their healthcare team to tailor these changes to their specific needs and circumstances.
How Long Does Juvenile Diabetes Treatment Take To Heal?
 It’s important to note that there is currently no cure for juvenile diabetes, also known as type 1 diabetes. Type 1 diabetes is a chronic condition in which the immune system attacks and destroys the insulin-producing beta cells in the pancreas. Since the body is unable to produce insulin, individuals with type 1 diabetes require lifelong insulin therapy to manage their blood sugar levels.
It’s important to note that there is currently no cure for juvenile diabetes, also known as type 1 diabetes. Type 1 diabetes is a chronic condition in which the immune system attacks and destroys the insulin-producing beta cells in the pancreas. Since the body is unable to produce insulin, individuals with type 1 diabetes require lifelong insulin therapy to manage their blood sugar levels.
While there is no cure for type 1 diabetes, advancements in diabetes management, including insulin delivery methods, glucose monitoring technologies, and research into potential treatments, have significantly improved the quality of life for individuals with the condition. The goal of treatment is to maintain blood sugar levels within a target range to prevent complications and promote overall health.
Individuals with juvenile diabetes need to work closely with their healthcare team to develop a personalized treatment plan that includes insulin therapy, regular monitoring of blood sugar levels, a balanced diet, and lifestyle modifications. Research is ongoing, and clinical trials exploring potential cures and innovative treatments continue to offer hope for the future.
Conclusion
In conclusion, juvenile diabetes treatment requires a holistic approach that encompasses insulin therapy, blood sugar monitoring, balanced nutrition, regular exercise, and emotional well-being. By embracing these lifestyle changes and leveraging advancements in diabetes care, individuals can lead fulfilling lives while effectively managing their condition. Remember, while a cure for type 1 diabetes is yet to be found, ongoing research and technology continue to pave the way for a future with improved treatment options and, hopefully, one day, a cure.
By staying informed, proactive, and resilient, those living with juvenile diabetes can navigate their journey with confidence and optimism, supported by a community that understands and empowers them every step of the way. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.