Welcome to our in-depth guide on managing Type 2 Diabetes Mellitus, a condition that affects millions worldwide. In this blog, we aim to empower those living with Type 2 Diabetes by providing a detailed roadmap for effective management of this chronic condition. We will explore the fundamental aspects of Type 2 Diabetes to explore the diabetes mellitus type 2 treatment options and lifestyle strategies.
Contents
What Are The Causes Of Diabetes Mellitus?
 Diabetes Mellitus, a group of metabolic diseases, is primarily caused by a combination of genetic and lifestyle factors. The causes can vary depending on the type of diabetes. Here’s an overview of the causes of Diabetes Mellitus:
Diabetes Mellitus, a group of metabolic diseases, is primarily caused by a combination of genetic and lifestyle factors. The causes can vary depending on the type of diabetes. Here’s an overview of the causes of Diabetes Mellitus:
- Autoimmune Reaction: The body’s immune system mistakenly attacks and destroys insulin-producing cells in the pancreas. The exact reason for this immune reaction is not entirely understood but is believed to involve a combination of genetic predisposition and environmental factors, such as viruses.
- Insulin Resistance: The cells in muscles, fat, and the liver start resisting or ignoring the signal that the hormone insulin is trying to send out—which is to grab glucose out of the bloodstream and put it into our cells.
- Genetics: A family history of diabetes can increase a person’s risk of developing the condition. Certain genetic markers are associated with an increased risk of Type 2 diabetes.
- Lifestyle Factors: Overweight, obesity, physical inactivity, and poor diet are significant risk factors for the development of Type 2 diabetes.
- Metabolic Syndrome: People with conditions like high blood pressure, abnormal cholesterol levels, high triglycerides, and abdominal fat are at increased risk.
- Hormonal Changes: During pregnancy, the placenta produces hormones that can lead to a buildup of glucose in the blood. Some women can’t produce enough insulin to handle this, resulting in gestational diabetes.
- Pancreatic Diseases: Conditions like pancreatitis, pancreatic cancer, and cystic fibrosis can damage the pancreas.
- Medications: Some medications, including steroids and antipsychotic drugs, can increase the risk of diabetes.
While genetic factors play a significant role in the development of diabetes, lifestyle choices are also critical. Especially in the prevention and management of Type 2 diabetes. Adopting a healthy diet and maintaining a healthy weight can significantly reduce the risk of developing this condition.
What Is The Best Diabetes Mellitus Type 2 Treatment?
The best Diabetes Mellitus type 2 treatment typically involves a combination of lifestyle modifications, medication, and ongoing monitoring. Here’s a detailed look at the treatment options:
Lifestyle Modifications
This involves a holistic approach focusing on diet, exercise, and overall wellness. A balanced diet, rich in nutrients, low in fat and sugars, and carefully managed in terms of carbohydrates, is crucial. Foods with a low glycemic index, such as whole grains, lean proteins, and plenty of vegetables, are recommended. Regular physical activity is equally important; engaging in at least 150 minutes of moderate aerobic activity per week can significantly improve blood glucose control, aid in weight loss, and boost overall heart health. Even a modest weight loss of 5-10% can lead to significant improvements in blood sugar levels.
Medications
When lifestyle changes are not enough to control blood sugar levels, medications are prescribed. Metformin is often the first medication used, known for its ability to improve insulin sensitivity and decrease glucose production in the liver. Sulfonylureas and meglitinides are used to stimulate the pancreas to produce more insulin. However, they differ in their duration of action and risk of causing low blood sugar. Thiazolidinediones work by increasing the body’s sensitivity to insulin. DPP-4 inhibitors help in subtly increasing insulin production and decreasing glucagon production. GLP-1 receptor agonists, often administered as injections, slow digestion and help lower blood sugar levels.
Insulin Therapy
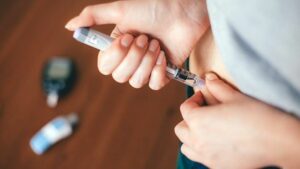 In some cases, especially where blood sugar levels remain high despite the use of oral medications, insulin therapy may be necessary. Insulin therapy involves injecting insulin to manage blood sugar levels. The type of insulin prescribed can vary, ranging from long-acting insulins that provide a steady amount of insulin throughout the day to rapid-acting insulins that are taken before meals to control the spike in blood sugar following eating.
In some cases, especially where blood sugar levels remain high despite the use of oral medications, insulin therapy may be necessary. Insulin therapy involves injecting insulin to manage blood sugar levels. The type of insulin prescribed can vary, ranging from long-acting insulins that provide a steady amount of insulin throughout the day to rapid-acting insulins that are taken before meals to control the spike in blood sugar following eating.
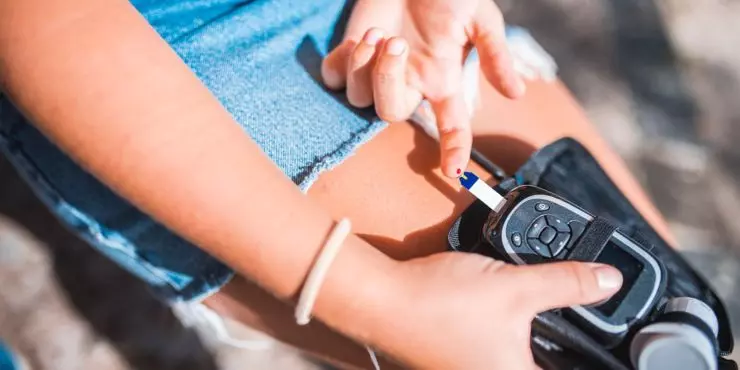
Regular Monitoring of Blood Glucose
Monitoring helps in determining how well the current treatment plan is working, understanding how diet, exercise, and stress affect blood sugar levels, and identifying low or high blood sugar levels before they become problematic. Self-monitoring of blood glucose (SMBG) is a common method where patients use a glucose meter to test their blood sugar. Continuous glucose monitoring (CGM) systems are also available, which provide real-time, dynamic glucose information throughout the day and night.
Managing Associated Conditions
Managing Type 2 Diabetes often involves addressing other related health conditions, primarily hypertension (high blood pressure) and dyslipidemia (abnormal cholesterol levels). Regular monitoring of blood pressure and lipid levels is essential. Medications such as ACE inhibitors or ARBs are commonly prescribed for hypertension in diabetic patients due to their additional kidney-protective effects. Statins may be prescribed for managing cholesterol levels.
Education and Support
Understanding the disease, its treatment, and how to manage daily life with diabetes is crucial for patients. Patient education programs often cover topics such as nutrition, exercise, medication adherence, blood sugar monitoring, and recognizing and handling episodes of hypo- or hyperglycemia. Support groups play a vital role as well, providing a platform for sharing experiences and strategies among peers, which can be incredibly empowering and encouraging. Additionally, psychological support may be necessary, as managing a chronic illness like diabetes can be overwhelming and lead to anxiety or depression.
Emerging Treatments and Research Frontiers
One area of advancement is in the development of new drug classes, such as non-insulin injectables that not only regulate blood sugar but also aid in weight loss and cardiovascular health. Research in insulin delivery methods is also progressing, including insulin pumps and the development of inhaled insulin. Another promising area is the field of pancreatic islet transplantation and stem cell therapy. This aims to restore insulin production in diabetic patients.
Each individual’s treatment plan should be tailored to their specific needs. And, regular consultation with healthcare providers is essential for optimal management.
Can You Manage Diabetes Mellitus Type 2 Without Insulin?
 Yes, Type 2 Diabetes Mellitus can often be managed without insulin, especially in its early stages or in less severe cases. The key is to focus on natural approaches that involve lifestyle modifications. Here are some of the most effective strategies:
Yes, Type 2 Diabetes Mellitus can often be managed without insulin, especially in its early stages or in less severe cases. The key is to focus on natural approaches that involve lifestyle modifications. Here are some of the most effective strategies:
- Low-Carb Diet: Reducing carbohydrate intake can help control blood sugar levels. Focus on low-glycemic foods like whole grains, legumes, nuts, seeds, fruits, and vegetables.
- Fiber-Rich Foods: High-fiber foods, such as vegetables, fruits, whole grains, and legumes, can slow the absorption of sugar and improve blood sugar levels.
- Aerobic Exercise: Activities like walking, swimming, or cycling can help the body use insulin more effectively and lower blood sugar levels.
- Resistance Training: Muscle-strengthening activities like weight lifting or yoga can improve blood sugar control and insulin sensitivity.
- Weight Management: Losing weight, particularly around the abdominal area, can significantly improve blood sugar control. Even a modest weight loss of 5-10% of body weight can have a substantial impact.
- Stress Management: High-stress levels can affect blood sugar levels. Techniques like meditation, deep breathing exercises, and mindfulness can help manage stress.
- Adequate Sleep: Good quality sleep is important. Poor sleep can affect blood sugar levels and insulin sensitivity. Aim for 7-8 hours of uninterrupted sleep per night.
- Herbal Remedies and Supplements: Certain herbs and supplements like cinnamon, berberine, and alpha-lipoic acid have been found to help improve insulin sensitivity and blood sugar control.
- Hydration: Staying well-hydrated helps kidneys flush out the excess blood sugar through urine.
- Avoiding Smoking and Limiting Alcohol: Smoking and excessive alcohol consumption can worsen the complications of diabetes.
It’s important to remember that while these natural approaches can be very effective, they should be implemented under medical guidance. Especially for individuals who are already on diabetes medication, as adjustments may be needed.
Conclusion
In conclusion, Diabetes Mellitus Type 2 treatment involves a comprehensive approach that includes lifestyle changes, medication, and regular health monitoring. By adopting a healthy diet, engaging in regular physical activity, and maintaining an optimal weight, individuals can significantly control their blood sugar levels. Medications, when necessary, play a crucial role, and staying informed about new treatments and technologies is beneficial.
Regular check-ups and monitoring for any complications are essential for overall health. Importantly, understanding the condition and having support can greatly enhance the effectiveness of management strategies. Do you want to get rid of diabetes? Join our online diabetes treatment program and reverse Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, Yoga, dieticians, and health coaches.